UTMB Neonatology Manual
Infectious Diseases
Infectious Diseases
THE MOTHER WITH AN INFECTION
1. A febrile, postpartum mother without a specific diagnosed site of infection can usually be allowed to handle and feed her newborn if she is feeling well enough, washes her hands thoroughly and wears a clean cover gown.
2. A mother with a respiratory tract infection should be informed that transmission of such infections on hands or fomites is common. She should be instructed in careful handwashing techniques and handling of items that might be contaminated with infectious secretions.
It might be wise for her to wear a surgical mask when she is with the baby to reduce the chance of droplet spread of infection.
3. Breastfeeding is usually possible even if the mother has one of many different overt infections or if she is receiving antibiotics. Breastfeeding is contraindicated in cases of:
a. Maternal AIDS or HIV infection
b. Maternal TB, untreated
c. Maternal varicella (if mother develops lesions in the 5 days before or up to 2 days after delivery).
4. A mother with a communicable disease that is likely to be transmitted to her baby should not have direct contact with the baby until the infection is no longer communicable. These include:
a. Maternal Rubella - until clear of rash
b. Maternal Gonorrhea - until treated for 24 hours
c. Maternal Rubeola - until clear of rash
d. Primary or Secondary Syphilis - until treated for 24 hours
e. Tuberculosis (Active) - until treated for 2 weeks
f. Maternal Varicella Zoster - until lesions are crusted
g. Maternal Hepatitis - until after the baby receives prophylaxis.
5. MRSA positive mothers. Infants born to MRSA-positive mothers will room in if medically feasible. When in the nursery, the baby will be under Contact Precautions. If the baby needs to undergo a special test or procedure (circumcision), this will be done using Contact Precautions.
Mothers colonized with MRSA may visit their newborn in the Nursery. The mother must visit only her baby and will be encouraged not to touch anything in the environment of the nursery. She may hold her baby after washing her hands and using a gown or barrier between her body and the baby's body. If an infant born to a MRSA-positive mother returns to UTMB within the first year of life, the infant will be admitted under Contact Precautions. The flag will be removed if the patient is cultured and found to be negative for MRSA or if the patient has not been in the hospital for the past year.
For other infectious conditions, refer to the appropriate section in this manual or the Red Book.
NEONATAL SEPSIS and OTHER INFECTIONS
Sepsis is defined as isolation of bacteria or other pathogenic organism from the blood of a baby with clinical signs. Proven sepsis in term infants is not common (1-2 per 1000 or 0.1%), but the diagnosis of suspected or clinical sepsis is made frequently. The incidence of proven sepsis is 20% in VLBW babies and up to 50% in the ELBW infant (less than 1000 g.). The high susceptibility of the developing fetus and newborn to sepsis is due to functional defects of both innate and adaptive immunity. These defects include immature cutaneous and mucosal barriers, low concentrations of T and B cells and lack of antigenic memory. Neonatal infections have been classified as early-onset (< 3 days of age), late-onset (>3-7 days of age) and very late onset (> 90 days of age). The definitions vary depending on the source of the literature, but the conclusions are generally comparable. Intrapartum prophylaxis for GBS has resulted in decreasing rates of early onset sepsis (EOS) for term infants. However, the incidence of non-GBS early onset sepsis is increasing for VLBW infants. Late onset neonatal sepsis (LOS) (from 8-90 days of life) affects two populations: healthy term infants in the community (which we will not discuss further) and preterm babies in the NICU - often referred to as nosocomial or hospital-acquired sepsis. Some experts consider infections acquired after 48-72 hours in the hospital to be hospital-acquired.
The signs of neonatal sepsis are extremely subtle in the newborn. Frequently, the nurse is the first to become suspicious and say "the baby is just not acting right." Clues include
Factors which place a neonate at increased risk for EOS include:
In VLBW infants, proven risk factors for LOS are:
Early newborn period (EOS)
Late newborn-neonatal period (LOS)
Based on consideration of all clinical factors, one must make a decision whether to observe the infant carefully, or culture and begin antibiotics. Preterm infants, especially those < 1500 g BW, should be treated more aggressively than a term baby.
The work‑up of an infant with suspected infection should include the following:
1. Examination with assessment of sensorium, tone, suck, and activity; review of vital signs
2. Review maternal history for risk factors and infections in the 2-3 weeks before delivery.
3. Complete blood count (CBC).
A recent large multi-center study of CBC in sepsis at < 3 days (EOS, n=166,092) found that WBC<8800, ANC<1533 and I/T > 0.24 were significantly associated with EOS; however, no single CBC index was both sensitive and specific in predicting positive blood cultures. No association was found between elevated WBC and EOS. Hornik CP, Benjamin DK, Becker KC et al. Use of the Complete Blood Cell Count in Early-onset Neonatal Sepsis. Pediatr Infect Dis J. 2012; 31: 799-802.
4. Blood culture(s)
5. Urinalysis (UA) and Urine culture in babies with presumed sepsis beyond 3 days of age. The genitourinary tract may serve as both a portal of entry for pathogens as well as a site of deposit for bacteria. The specimen should be obtained by bladder catheterization or suprapubic tap. But do not delay initiation of therapy while trying to obtain a satisfactory urine specimen.
6. Chest film. With chorioamnionitis due to prolonged rupture of membranes, intrauterine pneumonia is common. Pneumonia is frequently seen with GBS.
7. Rectal swab (if GI disturbances are present).
8. CSF culture. Because CNS involvement occurs in 25‑30% of babies with sepsis, CSF culture and examination for glucose, protein and cell count should be done unless the infant is clinically unstable, lumbar puncture is likely to cause further compromise, or initiation of antibiotic therapy will be delayed.
Cellular and chemical content of newborn CSF differs from that of older infants, as follows:
Examination of Cerebrospinal Fluid in Noninfected High-Risk Neonates*
|
Term Preterm ________________________________________________ White blood cell count (cells/mm3) Range 0-32 0-29 Mean 8.2 9.0 Protein (mg/dl) Range 20-170 65-150 Mean 90 115 Glucose (mg/dl) Range 23-119 24-63 Mean 52 50 Ratio of cerebrospinal fluid to blood glucose Range 44-248 55-105 Mean 81 74
|
|
* Modified from Sarff, L.D., Platt, L.H. and McCracken, G.H., Cerebrospinal fluid evaluation in neonates: Comparison of high risk infants with and without meningitis. J Pediatr. 88:473, 1976. |
In the first 72 hours of life, therapy should include ampicillin in combination with an aminoglycoside (Gentamicin). Initial therapy of suspected sepsis after 72 hours is usually vancomycin and gentamicin or cefotaxime.
The intravenous route should be used for therapy of meningitis or suspected sepsis. Duration of therapy for sepsis is 7‑10 days, and for neonatal meningitis, three weeks, or for two weeks after the spinal fluid becomes sterile ‑ whichever is longer. Dosages for commonly used antibiotics are summarized later in the chapter. Note that total dosage and intervals of administration vary with the postnatal age of the infant, the type of infection being treated, and in some instances the birth weight of the baby. (Source: Neofax, 2009).
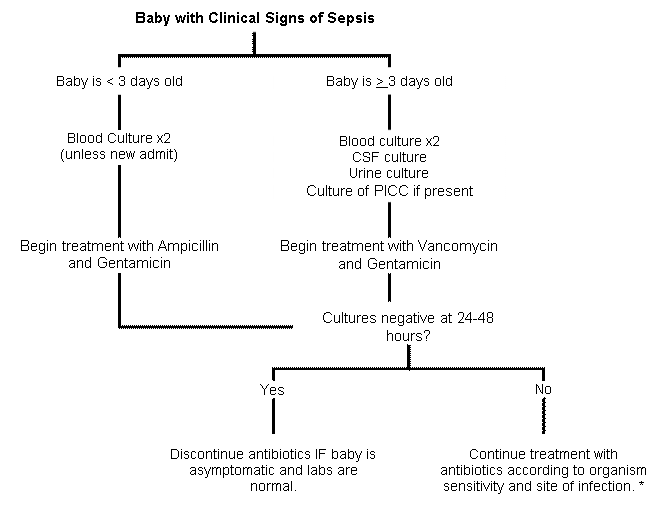
Recent data from UTMB in the term infant and from the literature in preterm babies support the discontinuation of antibiotics when the blood culture is negative at 24-36 hours, IF ALL OF THE CONDITIONS BELOW ARE MET:
days)
|
Murphy, Kara; Weiner, Joel. Use of Leukocyte Counts in Evaluation of Early-onset Neonatal Sepsis. Pediatr Infect Dis J 2012;31: 16-19. Background: Early-onset sepsis is a common diagnosis in neonatal intensive care units. Because of the low incidence, overtreatment is also common. Objective: To measure the sensitivity and negative predictive value of 2 serial white blood cell counts and a negative blood culture at 24 hours in predicting a noninfected neonate in the evaluation of early-onset sepsis. Methods: We performed a historical cohort study of neonates in the University of Massachusetts Newborn Nursery and neonatal intensive care unit born between 1999 and 2008 who had sepsis evaluations within the first 24 hours of life. Results: Three thousand two hundred thirteen patients were identified; 59 were excluded due to missing data. Of the 3154 included neonates, 1539 (49%) had 2 normal immature to total neutrophil (I:T) ratios and a negative blood culture at 24 hours. Normal I:T ratio was defined as <0.2. Two of these blood cultures showed growth of bacteria after 24 hours but were considered contaminants, and antibiotics were stopped at 48 hours. None of the 1539 neonates with normal I:T ratios was subsequently diagnosed with sepsis (negative predictive value 100%;95% confidence interval: 99.905% 100%). Conclusions: In this study, the combination of 2 serial normal I:T ratios and a negative blood culture at 24 hours in the evaluation of early-onset sepsis shortly after birth is indicative of a noninfected neonate. This suggests that antibiotics can safely be stopped at 24 hours in these neonates, which comprises approximately 50% of our study population. Key Words: early-onset sepsis, antibiotics, white blood cell count, I:T ratio |
Examples include the baby placed on antibiotics for what proved to be TTN, or the asymptomatic baby placed on antibiotics for a questionable CBC and GBS positive mother. If the baby is persistently symptomatic, preterm or there are other clinical concerns, continue the antibiotics.
Sepsis: Evaluation and Therapy in the Neonatal Nurseries Practice Guideline

*Two positive blood cultures are required for the diagnosis of CONS sepsis.
Usual duration of antibiotic treatment:
Group B b‑Hemolytic Streptococcus (GBS) Colonization and Disease
GBS are facultative diplococci which are subtyped into nine serotypes. Types Ia, Ib, II, III and V are the most common causes of neonatal disease. Type III is commonly associated with meningitis and late-onset GBS.
Pregnant women are colonized with GBS at rates of 15‑40%. Generally, they are asymptomatic but occasionally the organism causes postpartum infection with fever and sometimes systemic disease. Infection with GBS has been suggested as a cause of premature rupture of membranes, preterm labor, and postpartum fever. Higher colonization rates occur in women who are < 20 years old, primigravida, low socioeconomic status, or whose ethnicity is Hispanic, Caribbean, or African-American. Babies become colonized at birth or in utero or may become colonized nosocomially (neonate to neonate via hands of nursery personnel). It has been estimated that from 30‑70% of babies born to mothers with GBS will become colonized. However, early onset neonatal sepsis/meningitis or pneumonia has been found to occur in only about 1 baby per 100 colonized mothers.
Following is the algorithm used at UTMB for prevention of EOS in babies born to mothers with chorioamnionitis or colonized with GBS. It is modified slightly from the AAP/CDC guideline.(http://aapnews.aappublications.org/cgi/content/full/31/12/1,)
I. Mother GBS positive, and adequately treated, or treatment not indicated, specifically
-- Received penicillin, ampicillin, or cefazolin > 4 hours prior to delivery OR
-- No treatment and C-section delivery before onset of labor and with no membrane rupture prior to delivery:
Baby is term (> 37 weeks gestation):
Discharge at 24 hours (or with mother if C-section) IF access to medical care is readily available
Baby is preterm (<37 weeks gestation):
Observe in hospital for 48 hours (36 hours at discretion of the attending physician)
IIA. Mother GBS positive OR unknown with inadequate or no treatment prior to delivery and Baby is term (> 37 weeks)
Duration of membrane rupture <18h:
Observe in hospital for 48 hours (36 h at discretion of the attending physician)
Duration of membrane rupture >18h: CBC with differential at 6 hours of age
Observe in hospital for 48 hours (36 h at attending discretion)
IIB. Mother GBS positive OR unknown with inadequate or no treatment prior to delivery and Baby is preterm (<37 weeks)
CBC with differential at 6 hours of age
Observation in hospital for 48 hours (36 h at attending discretion)
III. Maternal chorioamnionitis, defined as her treatment with antibiotics during labor, regardless of GBS status or baby's gestation
CBC with differential at 6 hours of age
Observation in hospital for 48 hours (36 h at attending discretion)
IV. Maternal chorioamnionitis, defined as her treatment with antibiotics during labor, regardless of GBS status or baby's gestation, IF baby not well appearing
CBC with differential; Blood and CSF cultures (discuss with attending)
Antibiotic coverage
If baby appears sick, regardless of maternal GBS status, treat as appropriate cor clinical signs and symptoms.
Neonatal risk factors for early GBS infection include (each increases risk 5-35 fold): < 37 weeks gestation, ROM > 18 hours, mother with chorioamnionitis (chorio), bacteremia, or bacteriuria, multiple birth, heavy maternal colonization, < 20 years old.
In our ISCU, babies with GBS infections are placed on contact isolation however, this is beyond the recommendations of the AAP. Presently, there are no recommendations for treating colonized babies or hospital personnel since treatment has not been shown to reduce either maternal or neonatal disease. The current practice followed by UTMB obstetricians is to screen at 34-36 weeks for GBS, treat all mothers who are positive for GBS at delivery and treat all high risk patients in labor, i.e. those who have evidence of chorioamnionitis, are preterm, febrile, or have > 18 hours ROM.
Adequate treatment for maternal GBS is defined as one dose of penicillin, ampicillin, vancomycin or Cefazolin no less than 4 hours prior to delivery. Clindamycin is not considered to be adequate because of the high rate of resistance of GBS to this drug. However, at UTMB clindamycin is used only if GBS is sensitive; therefore, if the mother is treated with clindamycin and the GBS is documented to be sensitive, this is considered adequate treatmen
Treat GBS disease in the baby with ampicillin (200-300 mg/kg/day) or Penicillin G (250,000-450,000 units/kg/day), with the higher doses used for meningitis. Duration should be 10 days for sepsis, 14-21 days for meningitis, and 28 days for osteomyelitis. Bone and joint infections involving the hip or shoulder also require immediate surgical drainage, and the orthopedic surgeons should be involved as soon as the diagnosis is suspected.
Recurrent GBS disease occurs in 1-6% of cases. Repeat infection is treated similarly, but susceptibility testing is recommended. Recurrent GBS may be of a different strain. Rifampin is sometimes effective at eliminating mucus membrane colonization, but is less reliable than when used for meningococcemia prophylaxis.
Other Causes of Early Onset Neonatal Sepsis
Since the implementation of intrapartum antibiotic prophylaxis (IAP) against GBS, an increasing proportion of EOS cases are caused by E. coli and other gram-negative enteric organisms. Some, but not all, centers have reported increases in non-GBS EOS in preterm LBW infants.
Escherichia coli, particularly subtypes with the KI antigen, are the second most common organisms causing EOS. When E. coli sepsis/meningitis is suspected, a third-generation cephalosporin, such as Cefotaxime or Ceftazidime, should be added to the treatment regimen. Specific antibiotic therapy should be continued for 14 days in cases of E. coli bacteremia, and for 21 days in case of meningitis.
Next in frequency to GBS and E.coli are several gram positive organisms: Viridans streptococci (S. mitis, S. oralis, and S. sanguis), Group D Streptococcus (S. bovis), and Staphylococcus aureus. Most of the remaining infections in the United States are caused by Listeria monocytogenes or gram-negatives such as Klebsiella, Haemophilus influenzae, Enterobacter, Pseudomonas and Bacteroides fragilis.
Listeria monocytogenes are gram-positive, β-hemolytic rods which cause severe disease in pregnant women, their fetuses, in newborns and in the immune-compromised. Like GBS, it may be associated with both early and last onset disease. Incidence is 2-13 per 100,000 live births. Listeriosis is most commonly associated with ingestion of contaminated foods such as cheeses, deli meat and hot dogs. Infection may cause mild illness in a pregnant woman, but may result in spontaneous abortion or preterm labor.
EOS with Listeria is treated with ampicillin and gentamicin for 14 days; meningitis is treated for 21 days. Serial LPs are recommended until the CSF is negative.
Coagulase-negative staphylococci (CONS) account for almost half of LOS cases. Although rarely fatal or causative of site-specific disease, CONS often causes clinical instability associated with temporary cessation of feeds, increased respiratory support, longer hospitalizations, and poorer overall outcome.
Staphylococcus aureus is distinguished from CONS by the production of coagulase and by the presence of protein A in the cell wall. S. aureus causes bacteremia, meningitis, cellulitis, omphalitis, osteomyelitis and arthritis. Methicillin-sensitive S. aureus infections are treated with Nafcillin or Oxacillin, while methicillin-resistant staph (MRSA) requires treatment with Vancomycin. Additional therapy for persistent infection includes Rifampin, Linezolid or Daptomycin.
Enterococci (formerly Group D strep) are encapsulated organisms which produce biofilm and slime. Most enterococcal disease is associated with indwelling catheters and has low mortality. The treatment requires combined therapy of an aminoglycoside and Vancomycin or ampicillin. Vancomycin resistant enterococci (VRE) are an emerging problem.
Gram-negative organisms: LOS caused by E.coli, Pseudomonas aeruginosa, or Enterobacter has a high mortality rate (40-75%). Treatment of any of these bacteria requires two antibiotics.
Systemic Fungal infections: Disseminated neonatal candidiasis is usually caused by C. albicans or C. parapsilosis. Lethargy, increased apnea, feeding intolerance and poor perfusion are the common, non-specific clinical features of systemic candidiasis. Although thrombocytopenia is a consistent feature, it may not be found at presentation. Treatment is Fluconazole (10-12 mg/kg/day) or Amphotericin B (0.5 to 1 mg/kg/day) for 7-14 days. Meningitis should be treated with Flucytosine (5-FC) or Fluconazole. Further evaluation includes ultrasonography of the brain and kidneys to rule out abscesses, an eye exam to rule out endophthalmitis and an echocardiogram if a central line is in place to rule out catheter vegetations associated with endocarditis.
Malassezia furfur is a lipophilic dermatophyte which contaminates intravenous lipid preparations and frequently colonizes neonatal skin. Treatment consists of removing the contaminated catheter. Amphotericin B is indicated if the infection persists.
Focal skin infections such as cellulitis, pustulosis and omphalitis are usually caused by S. aureus.
Conjunctivitis refers to inflammation of the conjunctiva.
Gonococcal conjunctivitis presents with chemosis, lid edema and purulent exudates at 1-4 days of age. Gram stain and culture will confirm the diagnosis. Treatment is with ceftriaxone 25-50 mg/kg IV or IM (up to 125 mg). Babies should be evaluated for systemic disease.
Chlamydial conjunctivitis presents with inflammation, swelling and yellow discharge at 5-14 days of age. Diagnosis is made with ELISA or DNA probe testing of conjunctival scrapings. The treatment is erythromycin 40 mg/kg/day every 6 hours for 14 days. Babies should be evaluated for pneumonia.
Bacterial conjunctivitis, diagnosed by culture of eye exudates, may be caused by S. aureus, E. coli or H. influenza. Minor inflammation can be treated with erythromycin or gentamicin ophthalmic ointment. Severe cases may be associated with H. influenza or P. aeruginosa, and must be treated with parenteral antibiotics.
Herpes simplex virus may also cause conjunctivitis.
Pneumonia is a challenging diagnosis to make in the neonate. The typical clinical presentation may be indistinguishable from sepsis, and antibiotic treatment is similar. The usual patient is either a newborn in the first day of life with respiratory distress, or an older infant who is ventilator-dependent due to bronchopulmonary dysplasia. Most neonatal pneumonias are diffuse; focal opacifications on a chest radiograph are atypical, and should prompt a search for other causes. Respiratory management is discussed in the Pulmonary chapter.
Urinary tract infection may occur due to, or may cause, bacteremia. The incidence is higher in male infants, unlike older age groups. Gram negative organisms and enterococci are the most common causative organisms. Although urine culture is not needed in the work-up for EOS, it is very important in the evaluation of LOS. Diagnosis is made with urinalysis and a urine culture obtained by suprapubic bladder aspiration (SPA) or by catheterization. A positive urinalysis is defined as positive leukocyte esterase (LE) or microscopy positive for WBC or bacteria. Only urine obtained by SPA or catheterization is suitable for culture; a positive is defined as pure growth of more than 50,000 cfu/ml.
In the absence of other systemic disease, UTI is treated with antibiotics for 7-14 days. Prior to discharge, a renal ultrasound should be performed to rule out an anatomic cause of the UTI. VCUG should be performed after the second UTI or if renal ultrasound shows structural abnormality. It is more difficult to perform than renal ultrasound and is associated with complications such as bladder rupture. However, after the second UTI the risk of vesicoureteral reflux grade IV-V (hydronephrosis) increases markedly. (reference, UTI Clinical Practice Algorithm, Pediatrics, September 2011).
Prophylaxis for UTI, when appropriate, is Amoxicillin 10-20 mg/kg once daily. Depending upon the diagnosis, these patients should be seen by Urology or Nephrology after discharge.
Osteomyelitis and septic arthritis result either from hematogenous seeding in babies with bacteremia, or direct extension from a skin infection. Signs include localized erythema, swelling, pain on movement, or lack of spontaneous movement of the involved joint or extremity. The hip, knee and wrist are the usual joints involved. The femur, humerus, tibia, radius and maxilla are the bones most commonly affected.
S. aureus, GBS and gram-negative organisms are the typical causative organisms, so empiric treatment is with nafcillin, oxacillin, or vancomycin, and gentamicin.
Surgical drainage is often essential for infected joints, and orthopedic surgery should be consulted.
In the preterm baby, orthopedics should be consulted emergently because of the potential of irreversible damage to a septic joint. Duration of therapy is 3-4 weeks, ideally with an antibiotic known to be effective for the specific infecting organism.
Disability following osteomyelitis or septic arthritis can be significant due to the vulnerability of the growth plate at this age.
AMPHOTERICIN B
Indications: Systemic fungal infection
Dose and Interval: 0.5 to 1 mg/kg every 24 hours IV infusion over 2-6 hours.
Comments: Mix in D5W (precipitates in saline); concentrations should not exceed 0.1 mg/ml. Line should be flushed with D5W only, prior to administration. Incompatible with almost everything.
Toxicity: Nephrotoxicity (decreases renal blood flow and GFR), hypokalemia, hyponatremia, RTA, vomiting, chills, fever, anemia, thrombocytopenia, phlebitis. Monitor CBC, electrolytes, urine output, BUN and creatinine.
AMPICILLIN
Indications: Initial treatment of neonatal sepsis and meningitis; gram positive organisms (except penicillin‑resistant Staph); Listeria, H. influenzae, some E. coli.
Dose and Intervals: 25-50 mg per dose by IV slow push over 15‑30 minute infusion or I.M.
|
Postconceptual Age (weeks) |
Postnatal Age (days) |
Interval (hours) |
|
<29 |
0 to 28 > 28 |
12 8 |
|
30 to 36 |
0 to 14 > 14 |
12 8 |
|
37 to 44 |
0 to 7 > 7 |
12 8 |
|
≥45 |
All |
6 |
Comments: Toxicity rare; very large doses may result in CNS excitation or seizures.
CEFOTAXIME OR CEFTAZIDIME
Indications: Gram-negatives (E. coli, Klebsiella, H. influenza, Serratia, Proteus). Ceftazidime is preferred if P aeruginosa is strongly suspected and other gram positive antibiotic coverage is used.
Gonococcal infections: Cefotaxime 25 mg/kg per dose IV over 30 minutes, or IM.
Gonococcal prophylaxis for maternal gonorrhea: 100 mg/kg Cefotaxime over 30 min. or 1M.
Dose and Administration:
For cefotaxime: 50 mg/kg per dose IV infusion by syringe pump over 30 minutes, or IM.
For ceftazidime: 30 mg/kg per dose.
|
Postconceptual Age (weeks) |
Postnatal Age (days) |
Interval (hours) |
|
<29 |
0 to 28 > 28 |
12 8 |
|
30 to 36 |
0 to 14 > 14 |
12 8 |
|
37 to 44 |
0 to 7 > 7 |
12 8 |
|
≥45 |
All |
6 (Cefotaxime) 8 (Ceftazidime) |
Comments: Very few significant side effects have been reported, but may include rash, phlebitis, diarrhea, leukopenia, granulocytopenia and eosinophilia.
CLINDAMYCIN
Indications: Treatment of bacteremia, NEC with possible perforation, and pulmonary or deep tissue infections caused by anaerobic bacteria and some gram-positive cocci. Clindamycin should not be used in the treatment of meningitis.
Dosing and Administration: 5 to 7.5 mg/kg per dose IV over 30 minutes, or PO.
|
Postconceptual Age (weeks) |
Postnatal Age (days) |
Interval (hours) |
|
<29 |
0 to 28 > 28 |
12 8 |
|
30 to 36 |
0 to 14 > 14 |
12 8 |
|
37 to 44 |
0 to 7 > 7 |
12 8 |
|
> 45 |
All |
6 |
Comments: Monitor GI and liver status. Increase dosing interval in patients with significant liver dysfunction. Pseudomembranous colitis is most serious adverse effect.
FLUCONAZOLE
Indications: Treatment of systemic infections and severe superficial mycoses caused by Candida species which are unresponsive to amphotericin B.
Dose and Administration:
Systemic Infections: 12 mg/kg loading dose, then 6 mg/kg per dose IV infusion by syringe pump over 30 minutes, or PO.
Prophylaxis: 3mg/kg/dose IV
Thrush: 6 mg/kg on Day 1, then 3 mg/kg per dose q 24 hours PO.
|
Postconceptional Age (weeks) |
Postnatal Age (days) |
Interval (hours) |
|
< 29 |
0 to 14 > 14 |
72 48 |
|
30 to 36 |
0 to 14 > 14 |
48 24 |
|
37 to 44 |
0 to 7 > 7 |
48 24 |
|
> 45 |
All |
24 |
Comments: Serum fluconazole concentrations are not routinely followed. Assess renal function, AST, and ALT. Interferes with metabolism of barbiturates and phenytoin, and possibly theophylline.
GENTAMICIN
Indications: Initial treatment of newborn sepsis; gram-negative infections (proven or suspected).
Dose and Administration:
|
Postconceptual Age (weeks) |
Postnatal Age (days |
Dose (mg/kg/dose) |
Interval (hours) |
|
< 29* |
0 to 7 8-28 >28 |
5 4 4 |
48 36 24 |
|
30 to 34 |
0 to 7 >7 |
4.5 4 |
36 24 |
|
> 35 |
All |
4 |
24 |
|
* or significant asphyxia, renal dysfunction, PDA, or treatment with indomethacin |
|||
Administer by IV infusion by syringe pump over 30 minutes. (Administer separately from penicillin-containing compounds if serum drug levels are planned.). IV is the preferred route.
Gentamicin may be administered IM, but its absorption and blood levels may be erratic, particularly in VLBW babies.
Comments: Toxicity includes nephrotoxicity associated with prolonged high troughs and ototoxicity associated with prolonged high peak serum concentration.
Serum levels in term babies (> 37 weeks at birth). If renal status is stable, levels are not needed if therapy is given for 48-72 hours. For babies on longer courses of gentamicin therapy, obtain pre and post levels at the third dose (see below) and check serum levels 5 hours after the dose of gentamicin on about day 7, and weekly thereafter. Spot levels should be <2 mcg/ml.
Serum levels should be obtained in preterm infants as follows:
With IV administration, obtain initial levels at 3rd dose. Obtain trough level just before administering the 3rd dose and the peak 30 minutes after the end of a 30 minute infusion. Obtain levels earlier if the patient's renal status is unstable.
With IM administration, obtain levels around the 3rd to 5th dose. Obtain a trough level just before administering the drug and a peak level one hour after the dose. Trough levels should be <2 mcg/ml and peak levels should be 4-8 mcg/ml and < 10 mcg/ml. If adjustment of the dose is needed (based on the initial peak and trough), redraw levels only if gentamicin therapy will continue for more than four more days.
PENICILLINS
Aqueous (Crystalline) Penicillin G: IM or IV
Indications and Dosages:
GBS sepsis: 200,000 units/kg/day
GBS meningitis: 450,000 units/kg /day
Bacteremia (other than GBS): 25,000-50,000 units/kg per dose
Meningitis (other than Group B Strep): 75,000-100,000 units per dose IV over 30 minutes.
Congenital Syphilis (with or without CNS disease): 50,000 units/kg given every 12 hours (100,000 u/kg/day), for the first 7 days, then given every 8 hours for 7 days.
Dosing intervals:
|
Postconceptional (weeks) |
Postnatal (days) |
Interval (hours) |
|
<29 |
0 -14 >14 |
18 12 |
|
30 to 36 |
0-1 > 14 |
12 8 |
|
37-44 |
0-7 > 7 |
12 8 |
|
≥45 |
Any |
6 |
Procaine Penicillin G
For Congenital syphilis: 50,000 units/kg/day IM every 24 hours for 10‑14 days.
Benzathine Penicillin G
For congenital syphilis: 50,000 units/kg (one dose) IM
Comments: Very well tolerated. Low toxicity.
VANCOMYCIN
Indications: Methicillin‑resistant S. aureus, coagulase‑negative staph.
Dose and Administration: Initial empirical dosing: 15 mg/kg/dose for meningitis and 10 mg/kg/dose for bacteremia. Obtain serum trough level at the 3rd dose, just before administering the dose. Maintain trough serum levels of 5-10 mcg/ml. When treating MRSA pneumonia, endocarditis or bone joint infections consider troughs of 15-20 mcg/ml. Peak levels are needed only when treating meningitis; the level is obtained 60 minutes after the 60 minute infusion and the target is 30-40 mcg/ml. If adjustment of the dose is needed, redraw a trough level if vancomycin therapy will continue for more than 4 more days. Give IV over 60 minutes.
Toxicity: Nephrotoxicity and ototoxicity, which is enhanced by aminoglycosides; rash and hypotension (red man syndrome), neutropenia, and phlebitis.
CONGENITALLY ACQUIRED INFECTIONS
This chapter is intended only as a quick reference for the infections encountered most frequently in the nurseries. They are listed here in alphabetical order. Further reading is recommended when caring for a baby with any of these diseases, and consultation with the Pediatric Infectious Disease service may be required.
Human CMV is a DNA virus, and a member of the herpes virus group. Approximately 1% of all live-born infants are infected in utero and excrete CMV at birth, making this the most common congenital viral infection.
Clinical findings. Congenital CMV infections have a spectrum of manifestations. Usually infection is asymptomatic, but some congenitally infected infants who appear to be asymptomatic at birth are found in childhood to have hearing loss or learning disability.
Approximately 10% of infants with congenital CMV infection are symptomatic at birth. Infants may present with intrauterine growth retardation, neonatal jaundice, purpura, hepatosplenomegaly, microcephaly, brain damage, intracerebral calcifications, and chorioretinitis. Developmental delays are commonly found in later life. Sensorineural hearing loss (SNHL) is the most common sequela of congenital CMV, and it is more common in babies who have additional symptoms. CMV is the leading nongenetic cause of SNHL in the US; 21% of all congenital hearing loss (only half are symptomatic) and 25% of all hearing loss at age 4 years is attributable to congenital CMV.
33-50% of hearing loss from CMV occurs after infancy. In preterm infants, transfusion of CMV positive blood products has been associated with lower respiratory tract disease.
Vertical transmission of CMV to the infant occurs (1) in utero by transplacental passage of maternal blood-borne virus, (2) at birth by passage through an infected maternal genital tract, or (3) postnatally by ingestion of CMV-positive human milk. Infection acquired from maternal cervical secretions or human milk is usually not associated with clinical illness.
Severe sequelae are most likely from primary infection in the first half of gestation; however, in utero fetal infection can occur regardless of whether the mother had primary infection or reactivation during pregnancy.
Infants infected during maternal reactivation are much less frequently affected than those infected due to maternal primary infection, presumably because of immunity in the mother.
Diagnosis. In the asymptomatic baby, congenital CMV is usually diagnosed by isolation from the urine using polymerase chain reaction. CMV may be isolated from CSF in babies with CNS disease.
Treatment. In neonates with symptomatic congenital CMV disease of the CNS, ganciclovir, administered at 6 mg/kg/dose every 12 hours IV for 6 weeks, may protect against hearing deterioration and developmental impairment at 1-2 years. Preterm infants with pneumonitis, hepatitis or thrombocytopenia due to perinatally acquired CMV may be treated with ganciclovir for 2 weeks, assessed for improvement, and treated for an additional 1-2 weeks if deemed beneficial.
Control Measures. Neonates known to be CMV shedders excrete virus in urine and respiratory secretions. Particular attention to good handwashing techniques and the use of gloves when handling contaminated objects such as diapers is important, particularly in the ICU setting.
The etiologic agent of gonorrhea is Neisseria gonorrhoeae, a gram negative, oxidase positive diplococcus. Gonorrhea is most often an asymptomatic infection during pregnancy, but it may be associated with an increased risk of perinatal morbidity and mortality including fetal wastage, early and prolonged rupture of the membranes, and delivery of low birth weight babies. Intrapartum infection may result in disseminated disease with bacteremia, arthritis and meningitis, or scalp abscess if intrauterine fetal monitoring is done. Genital gonococcal (GC) infection is often associated with neonatal gonococcal ophthalmia.
Diagnosis of GC infection. The organism can be cultured or identified by nucleic acid amplification, using techniques such as PCR and transcription-mediated amplification.
Treatment of the Newborn.
Prophylactic Measures. Ophthalmic prophylactic treatment is administered routinely.Either 1% tetracycline ointment, or 0.5% erythromycin ointment (used at UTMB and most institutions in the US) is instilled into the eyes of every newborn during the transition period. Silver nitrate is no longer recommended for eye prophylaxis.
Asymptomatic babies born to mothers with recognized GC infection receive a single injection (IM or IV) of Ceftriaxone (25-50 mg/kg, not to exceed a total of 125mg). Topical prophylaxis alone is not adequate for these neonates, although GC ophthalmia rarely develops if prophylaxis is administered correctly.
Neonatal Ophthalmic or Disseminated Infections with GC.
For meningitis, therapy should be extended to 10-14 days. If the organism is sensitive to penicillin, treat with IV aqueous crystalline penicillin G at doses of 100,000 units/kg/day divided q 12 h, for 7-14 days
Hepatitis A (HAV). HAV infection is unusual in pregnancy and there is no chronic carrier state. Viremia and fecal shedding are short‑lived and usually absent or almost gone by the time symptoms appear, so infants born to mothers who have had acute disease are at minimal risk. Specific tests for antibody to hepatitis A (anti‑HAV) are available. IgM‑specific anti‑HAV signifies current or recent infection but may also occur during convalescence. The presence of IgG-specific anti-HAV signifies current or previous infection and indicates immunity.
Hepatitis A is not a neonatal problem unless the mother's symptoms begin between 2 weeks before and one week after delivery. In such cases a single injection of standard gammaglobulin, 0.02 ml/kg IM is recommended shortly after birth.
Hepatitis B (HBV). HBV infection occurs in 80‑90% of infants exposed to HbsAg/HbeAg positive mothers in the 3rd trimester or early postpartum period, and is detectable by 1‑4 months of age. Most infections are asymptomatic; rarely fulminant hepatitis occurs. About 90% of infected babies become chronic HBV carriers, with progression to chronic active hepatitis, cirrhosis, or hepatocellular carcinoma in 25%.
Below is a description of the hepatitis antigens and antibodies as they relate to infection:
Blood which is positive for HBsAg and HBeAg is highly infectious. Chronic infection is characterized by persistence of raised transaminase levels, HBsAg, HBeAg, and anti‑HBc. Most infants who are infected at birth become HBsAg positive within 4 months, but are usually negative at birth. This indicates that infection usually occurs around the time of delivery ‑ from swallowing amniotic fluid or maternal blood, leakage of virus across the placenta, or through minor abrasions at delivery. Babies born by c‑section are infected as readily as those born vaginally.
Management of HBsAg‑Positive Mothers and Their Infants. The neonate should be bathed carefully as soon as possible after birth to remove maternal blood and secretions. After bathing, the newborn does not require isolation or segregation from the rest of the babies.
Breastfeeding is permitted if the infant is appropriately immunized.
The concurrent use of HBIG and HB vaccine has an efficacy of about 90% in preventing chronic infection.The efficacy of HB vaccine alone, given at birth, and repeated at 3 and 6 months is about 75%. Preterm infants weighing < 2 kg whose mothers are HBSAg unknown or positive should receive HBlG and HBV at birth. They should start over routine 3-shot immunization at 2 kg.
HBV prophylaxis for the term infant whose mother is HepBSAg positive is summarized on the following table (see the "Red Book", for alternative scheduling):
|
AGE in mos. HBV Schedule HBV Marker Screening HB Vaccine** 1 mo HB Vaccine 6 mos. HB Vaccine HBsAg test *** 9 mos. HBsAg+ and anti‑HBs tests ++ *HBIG 0.5 ml IM within 12 hrs of birth **HB vaccine 0.5 ml IM within 7 days of birth and at 1 and 6 months ***Optional; if positive, indicates infection, and the third HB vaccine need not be given +If positive, indicates a therapeutic failure ++Anti‑HBs positive indicates a therapeutic success |
Hepatitis C (HCV). HCV is a small single-stranded RNA virus, a member of the Flavivirus family.
The prevalence of HCV infection in the US is estimated at 1.3%. Much like hepatitis A or B, hepatitis C is characterized by mild or asymptomatic infection with jaundice and malaise. Persistent infection occurs in 50-60% of infected children, and they are less likely to develop chronic hepatitis (70-80%) and cirrhosis than adults. HCV is the leading indication for liver transplantation for adults in the US. Vertical transmission is 5-6% and occurs only if the mother is positive to HCV RNA at the time of delivery; if the mother is also HIV positive, the risk of HCV transmission is higher. Breastfeeding does not increase the risk of HCV transmission.
At UTMB, the Pediatric Infectious Disease group has a protocol for follow-up of babies whose mothers have Hepatitis C.
If the mothers cannot return to UTMB for hepatitis C testing, written information must be given to her to review the need for hepatitis C testing with the primary care physician (PCP) of the baby at the very first clinic visit. The PCP will follow the testing protocol of his/her own preference. AAP guideline recommends early PCR at 1-2 months of age if 'desired, and to do hepatitis C antibody test at 18 months of age. Other published opinions are in favor of early PCR as a routine.
Most babies who are infected with herpes simplex virus (HSV) are born to mothers without a history of HSV. In newborn infants, HSV infection can manifest as 1) disseminated infection involving the liver and other organs, including the central nervous system (encephalitis); 2) localized central nervous system disease; or 3) disease localized to the skin, eyes, and mouth (SEM disease). Ocular manifestations include conjunctivitis, keratitis, and chorioretinitis. Of all cases of neonatal HSV, 20% are disseminated, ~33% are CNS, and the rest are SEM disease. Although common in older children, asymptomatic HSV infection occurs rarely, if at all, in neonates.
Typical vesicular skin lesions are helpful diagnostically, but they are only present in 60-75% of babies with disseminated or CNS disease, and in 80-85% of babies with SEM disease. Therefore, even if the pathognomonic skin lesions are absent, the differential diagnosis of respiratory distress, sepsis, and convulsions in newborn infants must include HSV infection. Initial symptoms can occur shortly after birth or as late as 6 weeks after birth. Disseminated and SEM diseases usually occurs during the first 2 weeks of life; disease localized to the central nervous system more often occurs during the second or third week.
Neonatal herpetic infections frequently are severe, with a high mortality rate and significant neurologic and/or ocular impairment of survivors, particularly in the absence of antiviral therapy. Recurrent skin lesions are often noted in surviving infants and are associated with sequelae if they occur frequently in the first 6 months.
The incidence of neonatal HSV disease ranges from 1 per 3,000 to 1 per 20,000 live births. Infants who develop HSV infection are significantly more likely to have been born prematurely and/or to be of low birth weight. 75% of neonatal infections are caused by HSV-2. HSV is most frequently transmitted to an infant during passage through an infected maternal lower genital tract during birth or by an ascending infection, sometimes through apparently intact membranes. Intrauterine infections causing congenital malformations have been implicated in rare cases. Less commonly, babies may be infected postnatally from the mother or father, usually from a nongenital infection, or from another infected infant, probably via the hands of personnel attending the infants. Postnatal transmission from personnel with fever blisters to neonates is extremely rare.
The risk of HSV infection in an infant born vaginally to a mother with a primary (first occurrence) genital infection is high (25% to 60%). The risk to an infant born to a mother with recurrent HSV infection at delivery is much lower- around 2%. Distinguishing between primary and recurrent HSV infection in women by history or physical examination may not be possible. Surveys suggest that 0.01% to 0.39% of American women shed HSV at delivery. Either primary or recurrent infection can be present in the mother without symptoms or nonspecific findings (e.g., vaginal discharge, genital pain, or shallow ulcers). Most infants (about 75%) who develop HSV infection are born to women without history or clinical findings suggestive of active infection during pregnancy.
Prevention of Neonatal Infections
Pregnant Women. All pregnant women should be questioned during a prenatal visit about history of HSV infection in themselves or in their sexual partners, and signs and symptoms of current infection should be sought as part of prenatal care.
Women in Labor. During labor all women should be questioned about recent and current HSV symptoms and carefully examined for evidence of genital HSV infection. Cesarean delivery of women in labor who have clinically apparent HSV infection (particularly primary infection) may reduce the risk of neonatal HSV infection unless the membranes have been ruptured for more than 4 hours. The risk in situations where the membranes have been ruptured for longer periods is uncertain, but many obstetricians prefer to deliver infants by cesarean section whenever the birth canal is infected regardless of membrane rupture.
A history of genital HSV for a woman in labor is not an indication for cesarean section. Scalp monitors should be avoided when possible in infants of women suspected of having genital herpes. The use of antiviral therapy in women with a history of HSV is unproven in efficacy and safety.
Infected Hospital Personnel. The risk of transmission to infants by personnel who have oral labial HSV infection ("cold sores") or who are asymptomatic oral shedders of the virus is not known, but probably is low. Personnel with cold sores who have indirect contact with infants should cover the lesions and avoid touching the sores. Of course they should also carefully observe handwashing policies, and must not kiss or nuzzle newborn infants or children with dermatitis. Personnel with herpetic whitlow should not have responsibility for direct care of neonates, immunocompromised patients, or patients in an intensive care unit.
Evaluation for Suspected HSV. Collect the following specimens for culture (best to place in viral transport media):
Symptomatic. Skin vesicles, mouth/nasopharynx/conjunctivae/anus (single swab), blood, and CSF. CSF should also be sent for routine indices and HSV PCR. Hepatic transaminases should be determined.
Asymptomatic. A swab specimen from mouth, nasopharynx, conjunctivae and anus can be obtained with a single swab ending with the anus and placed in one viral transport media tube. Full work-up should be done if the cultures are positive and treatment is initiated.
Care of Exposed Newborns
InfantsBorn to Mothers with Active Genital Lesions. The infant should be observed carefully for skin or scalp rashes, especially vesicular lesions, and unexplained clinical manifestations such as respiratory distress, seizures and signs of sepsis. If any of these occur, the infant should be evaluated for possible HSV as well as for bacterial infection. Skin lesions and a swab specimen as above should be cultured for HSV. Start Acyclovir if culture(s) from the infant are positive, if HSV infection is strongly suspected while awaiting culture results, if bacterial cultures are negative, or if no other cause of the infant's clinical manifestations is found.
Obtain HSV surface cultures as above for asymptomatic infants at 24 hours of age, since positive HSV cultures obtained at this time are more likely to indicate infection than transient colonization from intrapartum exposure. If surface cultures are positive, the baby should receive a full evaluation as for the symptomatic baby; if work-up is negative, the baby should be treated with acyclovir for 10 days to prevent HSV disease (2012 RedBook).
Infants Born to Mothers With History of Genital HSV but Without Active Lesions at Delivery.These infants should be carefully evaluated for clinical evidence of HSV. It is not necessary to obtain surface cultures in these babies routinely.
Treatment of Neonatal HSV infection.
Acyclovir is the treatment of choice for neonatal HSV infection. The dose is 60 mg/kg/d in 3 divided doses, given intravenously for 14-21 days, with the shorter duration used for SEM disease. Relapse of disease after cessation of treatment can occur and is usually related to host factors, but acyclovir resistance has been reported. Retreatment of infants with recurrent skin lesions is advisable due to association with CNS sequelae if occurring in 1st 6 months of life. Prolonged oral administration of acyclovir has been associated with neutropenia.
Infants with ocular involvement due to HSV infection should receive a topical ophthalmic drug (specifically, 1% trifluridine, 0.1% iododeoxyuridine, or 3% vidarabine), as well as parenteral antiviral therapy. Ophthalmologic consultation must be obtained.
All infants surviving neonatal herpes should receive 6 months of oral acyclovir suppressive therapy.
The best outcomes are associated with SEM disease. Most babies with CNS involvement have substantial sequelae, and the mortality of disseminated disease is 20%.
Control Measures and Isolation of the Hospitalized Patient
Neonates With HSV Infection or with positive cultures in the absence of disease, should be hospitalized in a private room, if possible, and managed with contact isolation as long as lesions are present.
Neonates Exposed to HSV During Delivery may be in the incubation phase of infection and should be carefully observed. One method of infection control is to have the infant room-in continuously with the mother in a private room. Infants born vaginally (or by cesarean delivery if membranes have been ruptured for more than 4 hours) to a mother with active HSV lesions should be physically separated from other infants and placed in contact isolation (and in an incubator) if they are hospitalized in the nursery during the incubation period.
Women in Labor and Postpartum Women with HSV Infection should be managed during labor, delivery, and the postpartum period with contact or drainage/secretion precautions, depending on the extent of the mucocutaneous disease. These mothers should be instructed on the importance of careful hand washing before and after caring for their infant. A clean covering gown may be used to help avoid contact of the infant with the lesions or infectious secretions. A mother with herpes labialis ("cold sores") or stomatitis should wear a disposable surgical mask when touching her newborn until the lesions have crusted and dried. She should not kiss or nuzzle her newborn until the lesions have cleared. Herpetic lesions on other skin sites should be covered. Breast feeding is acceptable if no lesions are present on the breast and if active lesions elsewhere on the mother are covered.
HIV type 1 (HIV-1) is an RNA retrovirus which requires the activity of a viral enzyme, reverse transcriptase, to convert the viral RNA to DNA, and is more common in the US than HIV-2.
Approximately 100-200 infants with HIV-1 infection are born annually in the US; mother-to child transmission of HIV-1 accounts for virtually all new infections in preadolescent children. The usual onset of symptoms is 12-18 months of age for untreated, perinatally infected children. HIV-positive mothers should not breast feed nor donate milk because HIV DNA has been detected in both the cellular and cell-free fractions of human breast milk. Transmission of HIV via breast milk has been documented (0.7%per month- this is true even if they have an undetectable viral load.)
Transmission/Incubation. The risk of infection for an infant born to an HIV-seropositive mother who did not receive preventive treatment is between 12% and 40%. Less than half of transmission events occur in utero; most occur during the perinatal period. The risk of transmission is decreased by cesarean section delivery.
Management of Infants Born to Mothers with HIV/AIDS. Standard precautions should be followed. The risk of transmission to healthcare personnel is minimal. The risk of HIV transmission to the newborn is significantly reduced by a maternal-newborn regimen of zidovudine. It is extremely important that a baby born to an HIV-positive mother be started on oral zidovudine (ZDV, or AZT) within 6-12 hours of birth. ZDV can be started before lab tests are drawn. For preterms <35 wks or babies who are NPO, consult with I.D. before beginning ZDV.
|
Dosing |
Duration |
|
|
Zidovudine |
≥35 weeks gestation:
Zidovudine should be started as soon after birth as possible and preferably within 6-12 hours of delivery
< 35 weeks gestation:
-- 1.5 mg/kg/dose IV q8h -- 2 mg/kg/dose PO q8h
-- 1.5 mg/kg/dose IV q8h -- 2 mg/kg/dose PO q8h |
Birth through 6 weeks |
|
2-drug regimen:
and Nevirapine |
Two drug regimen for high-risk neonates only Zidovudine: dose as above
Nevirapine Choose one of the following doses based on weight group, give as three doses, once on day 1, 3 and 7, as in the right side column: Birth weight 1.5-2 kg: 8 mg per dose give orally Birth weight >2 kg: 12 mg per dose given orally |
Zidovudine: Birth through 6 weeks
Nevirapine: 3 doses in the first week of life |
Diagnosis and Follow-up of HIV. See separate practice guideline.
The etiologic agent of syphilis is Treponema pallidum. Pregnant women should be screened with a serological test for syphilis (STS) at the first prenatal visit and then within one week of delivery. Both maternal results should be available before discharge of the infant.
The UTMB laboratory has recently changed to the syphilis IgG as a screening test for syphilis, which is confirmed with another specific treponemal test, the FTA‑ABS (Fluorescent Treponeme Antibody Absorption Test).
The RPR (Rapid Plasma Reagin) is used to determine titers if the treponemal tests are positive. Other hospitals and clinics may use the VDRL (Venereal Disease Research Laboratory). The RPR (or VDRL) tests for the presence of antibodies (IgG subclass) directed against the lipoidal antigen that results from interaction of body tissues with the spirochete when T.pallidum infection occurs. However, other diseases can cause this antigen to appear and stimulate antibody production. Some of these diseases include collagen vascular disorders, mononucleosis, tuberculosis, hepatitis, certain other viral infections as well as drug abuse. Therefore, a mother may have a positive RPR but may not presently have or have ever had syphilis (i.e., she has a biological false positive test.). A mother with a biologic false positive RPR will not have a positive FTA‑ABS, nor will her baby. Because the screening test for syphilis at UTMB is a treponemal test, we rarely see biologic false positive tests, but most centers begin with a non-treponemal test and confirm with a treponemal test.
With acquired syphilis, there may be a period of from 10‑90 days (mean 3 weeks) before the RPR becomes positive. With proper treatment the titer gradually decreases and after about 2 years the RPR usually reverts to negative. In contrast, the treponemal tests become positive early and stay positive for life in most people, despite adequate treatment.
Because the antibodies identified by the RPR and FTA-ABS or IgG tests are IgG antibodies, they readily cross the placenta. Therefore, a baby born to a mother who has active syphilis, treated syphilis, or biological false positive test will most likely have a positive RPR with a quantitative dilution titer about the same as that of the mother. Likewise, the baby of a mother with a positive FTA‑ABS will have a positive FTA‑ABS, so it is not useful to obtain an FTA-ABS on the baby.
The FTA‑ABS and IgG tests are qualitative tests and give results as either positive or negative. The RPR and VDRL are both qualitative and quantitative. The quantitative dilution titers are reported with positive tests. A titer of 1:32 or greater in the baby or a titer >4 times greater than the mother's titer is very suggestive of fetal infection. Note that the titers derived from the RPR or VDRL tests are not interchangeable. A reactive RPR with a titer of 1:16 is not comparable to a reactive VDRL with a 1:16 titer.
CSF serology is done using the VDRL while blood is used to do the RPR. FTA‑ABS is not done on CSF.
If the mother has a positive syphilis IgG, the clinical laboratory follows the algorithm below for further evaluation of the mother.
Neonatal Syphilis. A baby rarely has overt congenital syphilis at birth. The symptoms include snuffles, hepatosplenomegaly, rash, bullous eruption on palms and soles, lymphadenopathy, anemia, thrombocytopenia, conjugated hyperbilirubinemia, pneumonia, bone changes, fetal hydrops, and nephrosis/nephritis. More often babies return to the hospital at 2 to 3 weeks of age with these symptoms after having been sent home from the nursery where they were asymptomatic.
Evaluation of the ASYMPTOMATIC newborn with suspected syphilis (i.e., mother has a positive syphilis IgG assay and has not been treated) MUST include RPR on the baby's serum (titer of > 1:32 or > 4 times the mother's titer strongly suggests fetal infection), and a thorough maternal history which includes the dates of any previous serologic tests for syphilis, and the dates of any previous treatment.
The results of the baby's serum RPR and a thorough maternal history can be used to make further decisions.
The evaluation of the baby (and positive results of each study in parentheses) may include
1. Long bone x-rays (metaphysitis, trophic changes)
2. CSF evaluation for neurosyphilis: VDRL, protein (may be increased), cell count.
3. CBC (thrombocytopneia, anemia)
4. Liver function tests (elevated SGPT/SGOT, conjugated hyperbilirubinemia)
5. Ophthalmology consult (chorioretinitis)
At UTMB, the long bone films are the most likely part of the evaluation to be positive in the baby.
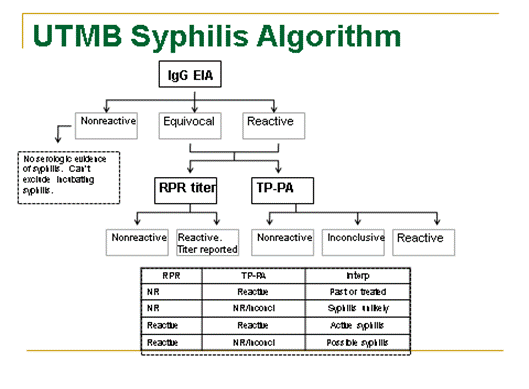
Management of the Asymptomatic Baby with Positive RPR and Mother with Positive RPR.
need to insert an image of this algorithm
Treatment of suspected congenital syphilis. For proven or probable congenital syphilis (based on the neonate's physical examination and radiographic and laboratory testing), the preferred treatment is aqueous crystalline penicillin G, administered intravenously. The dosage should be based on chronologic age rather than gestational age and is 50 000 units/kg IV, every 12 hours (1 week of age or younger) or every 8 hours (older than 1 week). Alternatively, procaine penicillin G, 50 000 units/kg, intramuscularly, can be administered as a single daily dose for 10 days; no treatment failures have occurred with this formulation despite its low CSF concentrations. When the neonate is at risk of congenital syphilis because of inadequate maternal treatment or response to treatment (or reinfection) during pregnancy but the neonate's physical examination, radiographic imaging, and laboratory analyses are normal (including infant RPR/VDRL either the same as or less than fourfold the maternal RPR/VDRL), some experts would treat with a single IM dose of benzathine penicillin G (Bicillin) at a dose of 50 000 units/kg. Most still would prefer 10 days of treatment. If more than 1 day of therapy is missed, the entire course should be restarted. Data supporting use of other antimicrobial agents (eg, ampicillin) for treatment of congenital syphilis are not available. When possible, a full 10-day course of penicillin is preferred, even if ampicillin initially was provided for possible sepsis. Use of agents other than penicillin requires close serologic follow-up to assess adequacy of therapy.
Infants who have a normal physical examination and a serum quantitative nontreponemal serologic titer either the same as or less than fourfold the maternal titer (eg, 1:4 is fourfold lower than 1:16) are at low risk of syphilis if (1) they are born to mothers who completed appropriate penicillin treatment for syphilis during pregnancy and more than 4 weeks before delivery; and (2) the mother had no evidence of reinfection or relapse. Although a full evaluation may be unnecessary, these infants should be treated with a single intramuscular injection of penicillin G benzathine, because fetal treatment failure can occur despite adequate maternal treatment during pregnancy. Alternatively, these infants may be examined carefully, preferably monthly, until their nontreponemal serologic test results are negative.
Minimal risk infants have a normal physical examination and a serum quantitative nontreponemal serologic titer either the same as or less than fourfold (eg, 1:4 is fourfold lower than 1:16) the maternal titer and (1) whose mother's treatment was adequate before pregnancy; and (2) whose mother's nontreponemal serologic titer remained low and stable before and during pregnancy and at delivery (VDRL less than 1:2; RPR less than 1:4) require no evaluation. Some experts, however, would treat with penicillin G benzathine as a single intramuscular injection if follow-up is uncertain.
Follow-up. All infants who have reactive serologic tests for syphilis or were born to mothers who were seroreactive at delivery should receive careful follow-up evaluations during regularly scheduled well-child care visits at 2, 4, 6, and 12 months of age. Serologic nontreponemal tests should be performed every 2 to 3 months until the nontreponemal test becomes nonreactive or the titer has decreased at least fourfold (eg, 1:16 to 1:4). Titers should decrease by 3 months of age and should be nonreactive by 6 months of age if the infant was infected and adequately treated or was not infected and initially seropositive because of transplacentally acquired maternal antibody. Patients with increasing titers or with persistent stable titers 6 to 12 months after initial treatment should be reevaluated, including a CSF examination, and treated with a 10-day course of parenteral penicillin G, even if they were treated previously.
Treponemal tests should not be used to evaluate treatment response, because passively transferred maternal treponemal antibodies can persist in an infant until 15 months of age. A reactive treponemal test after 18 months of age is diagnostic of congenital syphilis. If the nontreponemal test is nonreactive at this time, no further evaluation or treatment is necessary. If the nontreponemal test is reactive at 18 months of age, the infant should be evaluated (or reevaluated) fully and treated for congenital syphilis.
Treated infants with congenital neurosyphilis and initially positive results of VDRL tests of CSF or abnormal CSF cell counts and/or protein concentrations should undergo repeated clinical evaluation and CSF examination at 6-month intervals until their CSF examination is normal. A reactive result of VDRL testing of CSF at the 6-month interval is an indication for retreatment. Abnormal CSF indices that cannot be attributed to another ongoing illness also require retreatment. Neuroimaging studies, such as magnetic resonance imaging, should be considered in these children.
Management of Newborn Infant Whose Mother (or Other Household Contact) has Tuberculosis. Management of a newborn infant whose mother (or other household contact) is suspected of having tuberculosis is based on individual considerations. These infants should be reported to Hospital Epidemiology ASAP to assure home follow-up. If possible, separation of the mother (or contact) and infant should be minimized. The most commonly encountered circumstances are addressed below. Please see the Red Book for other situations:
Mother (or Other Household Contact) With a Positive Tuberculin Skin Test Reaction and No Evidence of Current Disease. A chest x-ray should be obtained on the mother. If mother has a negative CXR, no separation of mother and infant is necessary. Investigation of other members of the household or extended family to whom the infant may later be exposed is indicated. If no evidence of current disease is found in the mother or extended family, the infant should be tested with a Mantoux test (5 TU PPD) at 3 to 4 months of age should be done. When the family cannot be promptly tested, consideration should be given to the administration of INH (10 mg/kg/d) to the infant until skin testing of the family has excluded contact with a case of active tuberculosis. The infant does not need to be hospitalized during this time if adequate follow-up can be arranged. The mother is usually a candidate for INH preventive therapy.
Mother with Untreated (Newly Diagnosed) Disease or Disease Which Has Been Treated for 2 or More Weeks and Who Is Judged to Be Noncontagious at Delivery. Careful investigation of household members and extended family is mandatory. A chest roentgenogram and Mantoux tuberculin test should be done on the baby at 3 to 4 months and at 6 months. Separation of the mother and infant is not necessary if compliance with treatment for both mother and infant is assured. The mother can breastfeed. The infant should receive INH even if the tuberculin skin test and chest roentgenogram do not suggest tuberculous disease, since cell-mediated immunity of a degree sufficient to mount a significant reaction to tuberculin skin testing may develop as late as age 6 months in an infant infected at birth. INH can be discontinued if the Mantoux skin test is negative at 3 to 4 months of age and no active disease exists in family members. The infant should be examined carefully at monthly intervals. If noncompliance is documented, the mother has AFB-positive sputum (or smear), and supervision is impossible, BCG (Bacillus Calmette-Guerin) vaccine may be considered for the infant. However, the response to the vaccine in infants may be inadequate for prevention of tuberculosis.
Mother Has Current Disease Suspected of Being Contagious at the Time of Delivery (abnormal CXR or evidence of active disease). The mother and infant should be separated until the mother is judged to be noncontagious, then proceed with management as in the preceding paragraph.
Epidemiology is summarized as follows:
Fetal Exposure in Early Gestation: The risk of Varicella embryopathy (congenital varicella) is 2%. Symptoms include scarring of the skin in a dermatomal distribution, limb atrophy with bone and muscle hypoplasia, ocular defects (cataracts, microphthalmia, chorioretinitis), and neurological abnormalities (mental retardation, microcephaly, dysfunction of bowel and bladder sphincters). Embryopathy does not require treatment with VZIG or isolation.
Fetal-Newborn Exposure in Late Gestation: If the mother develops varicella from 5 days before to 2 days after delivery, the newborn is at high risk of fulminant severe infection, with high mortality (30%). The baby develops varicella between 1 and 16 days of life (usual time from onset of rash in the mother to onset in the neonate is 9-15 days).
Treatment of the baby: Place in strict isolation, and if remains hospitalized, for up to 21 days (28 days if received VZIG). Administer VZIG, 125 units I.M. as soon as possible after delivery (for maximal effectiveness, give within 48 hours and not more than 96 hours after exposure). About 50% of babies who receive VZIG will develop varicella.
Postnatal Exposure, other than as discussed above, is not a problem for healthy term infants. VZIG is not indicated.These babies are at no greater risk for complications of chickenpox than are older infants and children. In the hospitalized population, VZIG is indicated for all preterm babies <28 weeks gestation or <1000g BW and for preterms >28 weeks gestation whose mothers have a negative history of infection. If an exposure occurs within the hospital, identify susceptible patients and give VZIG. The exposed personnel must follow airborne isolation procedures or stay away from work from 8-21 days after their exposure to varicella.
Isolation of the Hospitalized Patient. Airborne precautions must be followed. Establishment of the date of rash onset is key. For the index case, the patient must be isolated for 5 days from rash onset or duration of vesicular eruption (whichever is longer). Exposed patients must be isolated for 8-21 days after onset of rash in the index patient.