Clinical Assessment of Dehydration
Clinical assessment of dehydration is always approximate, and the child should be frequently re-evaluated for continuing improvement during correction of dehydration.
| Mild | Moderate | Severe | |
|---|---|---|---|
| Weight loss for infants | Up to 5% | 6-10% | 10-15% |
|
Weight loss for children |
Up to 3% |
6% |
9% |
| Appearance | Active, alert | Irritable, alert, thirsty | Lethargic, looks sick |
| Capillary filling (compared to your own) | Normal | Slightly delayed | Delayed |
| Pulse | Normal | Fast, low volume | Very fast, thready |
| Respiration | Normal | Fast | Fast and deep |
| Blood pressure | Normal | Normal or low Orthostatic hypotension | Very low |
| Mucous memb. | Moist | Dry | Parched |
| Tears | Present | Less than expected | Absent |
| Eyes | Normal | Normal | Sunken |
| Pinched skin | Springs back | Tents briefly | Prolonged tenting |
| Fontanel (infant sitting) | Normal | Sunken slightly | Sunken significantly |
| Urine flow | Normal | Reduced | Severely reduced |
When we talk of "5% dehydration", it means that the child has lost an amount of fluid equal to 5% of the body weight. If you have an accurate pre-illness weight, you may use that weight. Alternatively, the pre-illness weight can be calculated as follows:

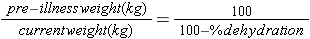
So,
- A 10 kg child who is 5% dehydrated will weigh 9.5 kg.
- A 10 kg child who is 10% dehydrated will weigh 9 kg.
- A 5 kg child who is 10% dehydrated will weigh 4.5 kg.
The child's current (dehydrated) weight can be used for calculation of dehydration and maintenance fluids. After all, clinical assessment of dehydration, and therefore the volume needed for correction, is approximate!

