 ER Nurse Kelly Ferguson (right) with former preceptor, ER Nurse Emily who impacted her decision to join the ER department.
ER Nurse Kelly Ferguson (right) with former preceptor, ER Nurse Emily who impacted her decision to join the ER department.
When most people think of an emergency room, they probably picture ambulances with blaring sirens rushing up to the ER carrying patients with bloody bodies. They may envision a man clutching his chest from heart attack pain, as he’s rushed through the halls on a stretcher.
Well at least that’s what I imagine. And if that’s also what comes to mind for you, think again.
I recently spent time with ER Nurse Kelly Ferguson who gave me a totally different view of one of the hospital’s most popular departments.
Ferguson is not only a UTMB employee but an alumnus of the School of Nursing, which is what brought the soon-to-be mother of two to the hospital.
“I decided to work in the UTMB ER after completing my capstone, here in the ER department,” she said. “I fell in love with it and I love that UTMB is a teaching hospital as well.”
When I meet up with Ferguson she’s half-way through her 12-hour shift. “It’s unusually slow today,” she explains, apologetically. “I don’t think you’ll get a true feeling of the ER today.” I tell her that’s OK, since I hadn’t had a V8 and didn’t quite have the energy for a trauma-filled experience. But Ferguson quickly dispels that myth.
“Most of the people who come into the ER are not in a life or death situation,” she said. “A lot of what we see is acute care and not a true emergency.”
Ferguson’s day began at 6:45 a.m. When she started her shift, the ER had only three patients, so she was assigned to be a “float nurse” for the morning.
She explains that the ER is divided into units: triage, trauma, META (minor emergency treatment area), the rapid decision unit, surge and the main ER. Usually an ER nurse is assigned to a unit, but because it’s a slow morning so she will “float” or move throughout all units.
Before she begins in the triage unit, where patients are initially assessed when 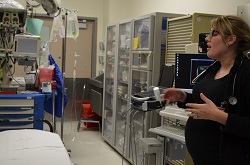 they enter the ER, she restocks supplies in the patient rooms.
they enter the ER, she restocks supplies in the patient rooms.
By 8 a.m. she relieves a nurse who is going on break and assesses an elderly patient. His wife brought him in, stating he was showing confusion that morning, asking for his deceased mother. Ferguson refers to his condition as an altered mental status. She performs an electrocardiogram, to make sure the patient hasn’t had or isn’t having a heart attack and asks for his medical history. She discovers that he recently started a new medication and suspects this may be the cause of his confusion.
By 8:45 a.m. she has moved on to her second patient, a man having difficulty urinating. Per the attending physician’s orders she takes the patient’s blood.
The ER is still slow so Ferguson doesn’t see her next patient until 11 a.m., when she’s assigned to the surge unit, where she will spend the rest of her day.
The 80-something year-old patient was sent to the ER from UTMB’s physical therapy department due to elevated blood pressure.
By around 2 p.m., the patient load picks up some and I get to see Ferguson in fast-paced ER action. “I’m assigned these four exam rooms,” Ferguson said as she points to four adjacent patient rooms.
She moves from room to room assessing patients, effortlessly and gracefully at a fast-paced speed — all while six months pregnant, let me not forget to mention. And if I’m not careful, I may actually get left behind. OK, I actually do a few times, but don’t judge me.
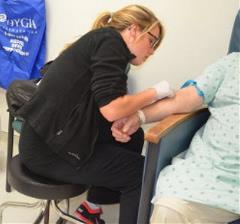 I’m impressed by Ferguson’s medical insight as she questions a young male complaining of shortness of breath. She asks detailed questions to get a full picture of his problem and the possible cause. She quickly grabs her stethoscope to listens to his lungs. Not missing a beat, or should I say symptom, she asks the patient about a scar on his ear. He says it’s cancer that has spread to his lungs, a detail he had yet to mention.
I’m impressed by Ferguson’s medical insight as she questions a young male complaining of shortness of breath. She asks detailed questions to get a full picture of his problem and the possible cause. She quickly grabs her stethoscope to listens to his lungs. Not missing a beat, or should I say symptom, she asks the patient about a scar on his ear. He says it’s cancer that has spread to his lungs, a detail he had yet to mention.
She quickly goes back to her station to key in his history in his electronic chart, which will then go to the attending physician who will decide on the next course of action.
Then she’s quickly off to her next patient. And this is when things really get interesting.
A patient is brought in by ambulance as a recent release from the Texas City jail. I enter the patient exam room with caution, given his recent incarceration, but Ferguson isn’t jaded by his recent run-in with the law.
She’s not moved by his blood-stained clothes and two black eyes, which the patient attributes to an altercation with the police two nights prior. Meanwhile, I’m wondering if we need security, but that’s why she’s a nurse and I’m not, because Ferguson isn’t the least bit bothered.
She treats the patient with the same respect as any other and begins a quick yet thorough assessment. She gathers that he’s come in for elevated blood pressure, a result of being off his medication while incarcerated.
She quickly moves back to her station to put notes in his electronic chart and then draws a blood sample from the cancer patient.
As Ferguson returns to the station to input notes, the physician informs her that the recently released “jail patient” has removed his IV.
Before going back to check on him, however, Ferguson attends to her elderly patient per the prompting of a fellow nurse who has noticed a change in his behavior that could be indicative of a stroke.
The nursing unit works together as a team.
After taking the elderly patient’s pressure, Ferguson goes back to check on the recently released jail patient and cleans up his arm from where he’s removed his IV. Then she quickly moves back to the station to input notes, while receiving an order to get a blood sample from the elderly patient.
And while Ferguson is with the elderly patient, the “jail patient” sneaks away. We discover this fact after returning to the station and the doctor informs us that he has gone missing after asking to use the restroom.
Ferguson isn’t surprised and explains that it’s common for the ER to receive  patients from local jails who then leave the ER before being properly treated.
patients from local jails who then leave the ER before being properly treated.
After three patient assessments, six patient check-ins, three blood draws, three blood pressure readings, and six chart notes within 45 minutes, Ferguson still apologizes for it being slow. Whew!
Shortly after discharging the AWOL “jail patient,” Ferguson’s charge nurse sends her home for the day due to the low patient census.
But before she leaves, Ferguson tells me more about her work life in the ER.
“I feel the work I do is fulfilling UTMB’s mission to improve health for the people of Texas and around the world,” she said. “I know it sounds cheesy but we do save lives.”
“No one wakes up and thinks I’m going to be in the ER today,” said Ferguson. “But I count it as an honor to be in someone’s life when they’re at their worst.”
And that’s a day in the life of an ER nurse. And you’re not cheesy, Ferguson. There’s nothing cheesy about saving lives. Hats off to you!