“
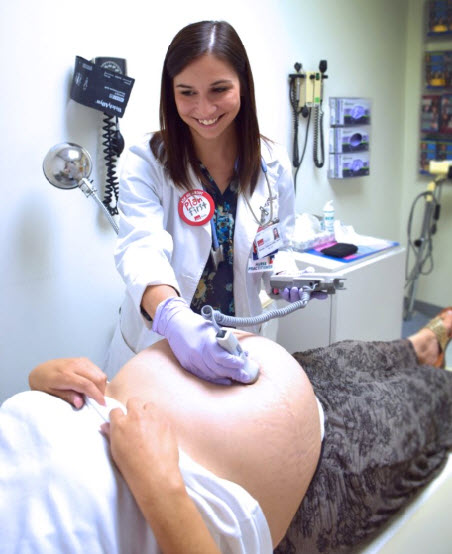
How are you feeling? Is the baby moving? Any contractions?”
It’s not even 8:30 a.m. and Kirsten Emanuel, a nurse practitioner specializing in women’s health and OB-GYN at the Regional Maternal and Child Health Clinic in Conroe, is already on her fourth patient of the day.
“My average for last month was 23 patients a day, so that’s a lot,” said Emanuel. “On my schedule today, I still have three prenatal visits, then a new obstetrics visit, a family planning visit and a three-week postpartum visit—all before noon.”
At 26 years old, she is the youngest NP in the building and radiates energy and enthusiasm when she talks about her job, which she’s held for the past year and a half.
“I get ‘How old are you?’ at least twice a day,” Emanuel says. “But then, as soon as I start talking and explaining things, I get ‘Oh, she knows what she’s talking about’ (laughs). But seriously, I feel like I’m making a difference—and I have a big heart for the younger population. I try to make them really comfortable and explain everything to them. We do a lot of family planning and try to prevent unexpected pregnancies by educating young women about family planning options and birth control methods that are available.”
 Her clinic in Conroe is one of 13 in UTMB’s Regional Maternal and Child Health Program, dedicated to providing high-quality, low-cost health care to eligible women and their families. Spread across East and Southeast Texas, the RMCHPs offer a wide variety of services, including family planning, prenatal care, and breast and cervical cancer screening.
Her clinic in Conroe is one of 13 in UTMB’s Regional Maternal and Child Health Program, dedicated to providing high-quality, low-cost health care to eligible women and their families. Spread across East and Southeast Texas, the RMCHPs offer a wide variety of services, including family planning, prenatal care, and breast and cervical cancer screening.
The expansive regional network also consists of 22 WIC (Women, Infants and Children’s nutrition program) sites, some co-located with clinics. Together, they fill a crucial gap for the underserved population, with close to 300,000 clinic patient visits and WIC client visits a year.
On my drive up to Conroe, which is about 45 minutes north of Houston, I wasn’t sure what to expect, since I had never visited an RMCHP. I was prepared to see a busy waiting room, but didn’t fully grasp how many people are served each and every day until I walked into the lobby area—it was completely full of pregnant women, parents and young children, with no seats to spare. A Disney movie provided entertainment for little ones while parents filled out paperwork and waited for their name to be called.
Emanuel emerged from behind the clinic door to lead me back to her office. She had just finished a postpartum followup appointment and was busy charting and reviewing the medical history of her next patient, who had just arrived.
I follow her as she walks into a room where a 19-year-old who is 34 weeks pregnant is waiting along with her mom. The young woman is diabetic and has been coming to the clinic twice a week for evaluation.
Emanuel asks the patient how her week is going as she hooks her up to a fetal monitor for an NST, or non-stress test, which monitors the baby’s heart rate. During the visit, Emanuel grows concerned about the patient’s high blood pressure.
After consulting with her clinic manager, Emanuel advises the young woman to drive to UTMB’s John Sealy Hospital in Galveston for additional monitoring.
“A lot of the patients we serve are high risk and have comorbidities, such as diabetes and high blood pressure, which can complicate the pregnancy,” said Emanuel. “I don’t accompany my patients to Galveston, but I call to let the hospital know when a patient is on her way. Once they arrive at JSH, all their charting and medical information is already there for the physicians.”
Emanuel explains that most of her patients travel to Galveston to give birth, as well.
“If there is an emergency, we send our patients to the nearest hospital, but we explain that UTMB is the best place to deliver,” said Emanuel. “At 28 weeks, we start talking about delivery and make sure someone is available to bring them to Galveston for a scheduled C-section or induction. It’s fun for me to see patients all the way through their pregnancy and then follow up with them afterward. I usually call my patients when they get down there to see how they are feeling, and I try hard to make them feel like I’m there for them.”
 Whether it’s in English or Spanish, Emanuel has learned to explain plans of care
Whether it’s in English or Spanish, Emanuel has learned to explain plans of care
to her patients. She welcomes her next two patients in Spanish, immediately setting them at ease.
“The majority of our patients speak Spanish, so I’ve had to pick it up,” said Emanuel. “All of our clinical and clerical staff is bilingual, too, so if there’s something I really need to get across or a patient is looking at me with a blank stare, I can go get one of our staff members to help translate.”
After talking to a pregnant patient from Venezuela about scheduling an induction date, Emanuel gets a translator to make sure the patient understands where and when to go to Galveston, and what to expect.
Emanuel smiles and says that she still needs to work on her Spanish.
“I made this woman a baby blanket because she didn’t have anything at home for a newborn,” said Emanuel. “When she came in for her postpartum follow-up, she was speaking in Spanish and I didn’t fully understand what she was saying, but answered ‘Si, gracias.’ After the patient left , one of my colleagues informed me that I had unknowingly agreed to be the baby’s godmother!”
I stick around as Emanuel visits with two more patients. While she doesn’t have any time to waste, she sits down with each woman and listens to her questions and concerns without seeming like she’s in a rush—and to do that more than 20 times a day shows how much she genuinely cares for each and every person.
“It’s hard work and it isn’t easy to do this day in and day out, but I also have the chance to make a difference and that’s the best part of my job,” said Emanuel.