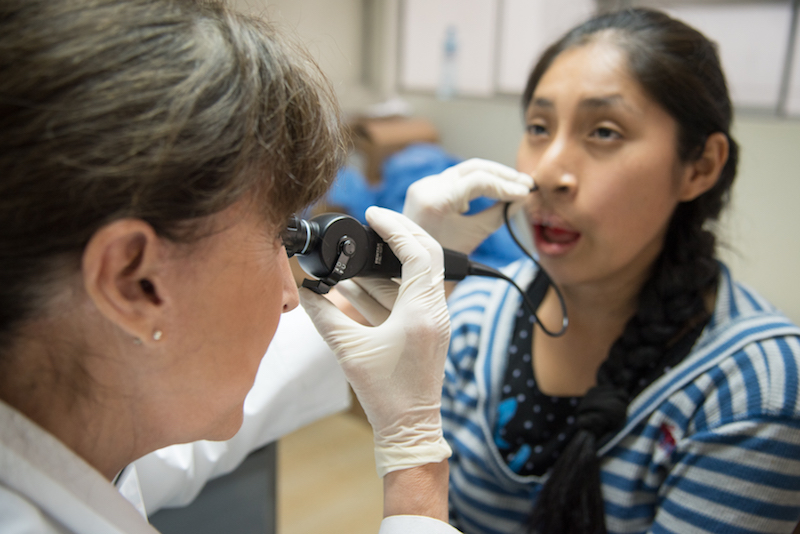
 Salas-Provance uses an endoscope to examine the throat of a patient with pervasive hypernasality, which makes it difficult to speak normally.
Salas-Provance uses an endoscope to examine the throat of a patient with pervasive hypernasality, which makes it difficult to speak normally.
There’s a photo on Marlene Salas-Provance’s desk that shows her standing next to a tired but grateful-looking father and a smiling young girl. It’s a daily reminder of the important work she does around the world.
“The father and his young daughter lived in extreme poverty high up in the Andes. They traveled for three days—walking, hitching rides, by boat—to get to La Oroya, Peru, so his daughter could get cleft palate surgery,” said Salas-Provance, PhD, a speech pathologist who joined UTMB in May as associate dean for Academic and Student Affairs in the School of Health Professions.
For the last 11 years, Salas-Provance has traveled to Peru, China, the Philippines, El Salvador, Venezuela and the Dominican Republic with Rotaplast International, a nonprofit organization that provides free reconstructive surgery and treatment to those with cleft lip and palate.
Most recently, Salas-Provance returned from Lima following a two-week mission, where she worked with an interdisciplinary team to educate, evaluate and perform surgeries on children and adults with orofacial clefts. These birth defects occur when a baby’s lip or mouth do not form properly during pregnancy and can result in problems with feeding and speaking clearly. Peru has a high rate of cleft lip and palate, occurring in approximately one of every 500 births.
“My role was to provide speech assessments and parent/patient education regarding the development and improvement of speech. On my first day, I screened more than 100 patients,” said Salas-Provance. “I also performed 30 nasal endoscopy exams, where I look at the closure patterns of the muscles in the velopharyngeal area. If the muscles can’t close all the way, a person can’t build up air pressure in the mouth because air escapes out of the nose—that can make speech difficult. Based on what I saw, I worked with the plastic surgeons to select the most optimal type of surgery for each patient.”
In addition, she offered guidance on adapted feeding techniques for babies with cleft lip and palate and assisted the team dentist with building prosthetic devices to improve the speech of adults who were not good candidates for surgery.

Salas-Provance has a close connection to two speech pathologists, an orthodontist and prosthodontist in Peru, and will refer patients to them as necessary to ensure they receive continuity of care. Speech therapy is an important part of the process, especially after surgery.
“The longer a person has a mechanism that doesn’t function, the more ingrained the errors for speech become and then the speech pathologist has to untangle all of that once the musculature is intact,” said Salas-Provance. “I’m bilingual and speak Spanish so I can talk with families about what they need to do for their children in terms of speech development and connect them with colleagues in Peru for therapy following the surgery. During these mission trips, we work 12 hour days, but I love it. It’s satisfying for me, and families are so appreciative.”
Salas-Provance has been back to Peru seven times and has seen many of the same patients, who now have the opportunity to find employment and marry as adults.
“There’s a huge psychosocial aspect to appearance,” she said. “If you look nice and talk normal, people tend to be more accepting of you as an individual. You’re more likely to get an education, a job—everything.”
Since coming to UTMB from New Mexico State University, Salas-Provance has been looking for a cleft-palate team to join in Galveston. She plans on continuing to help transform lives around the world, and hopes to take SHP students with her in the future.
“The difference you make is huge. A child’s life is changed forever” said Salas-Provance. “It’s a very manageable fix with a very significant outcome.”