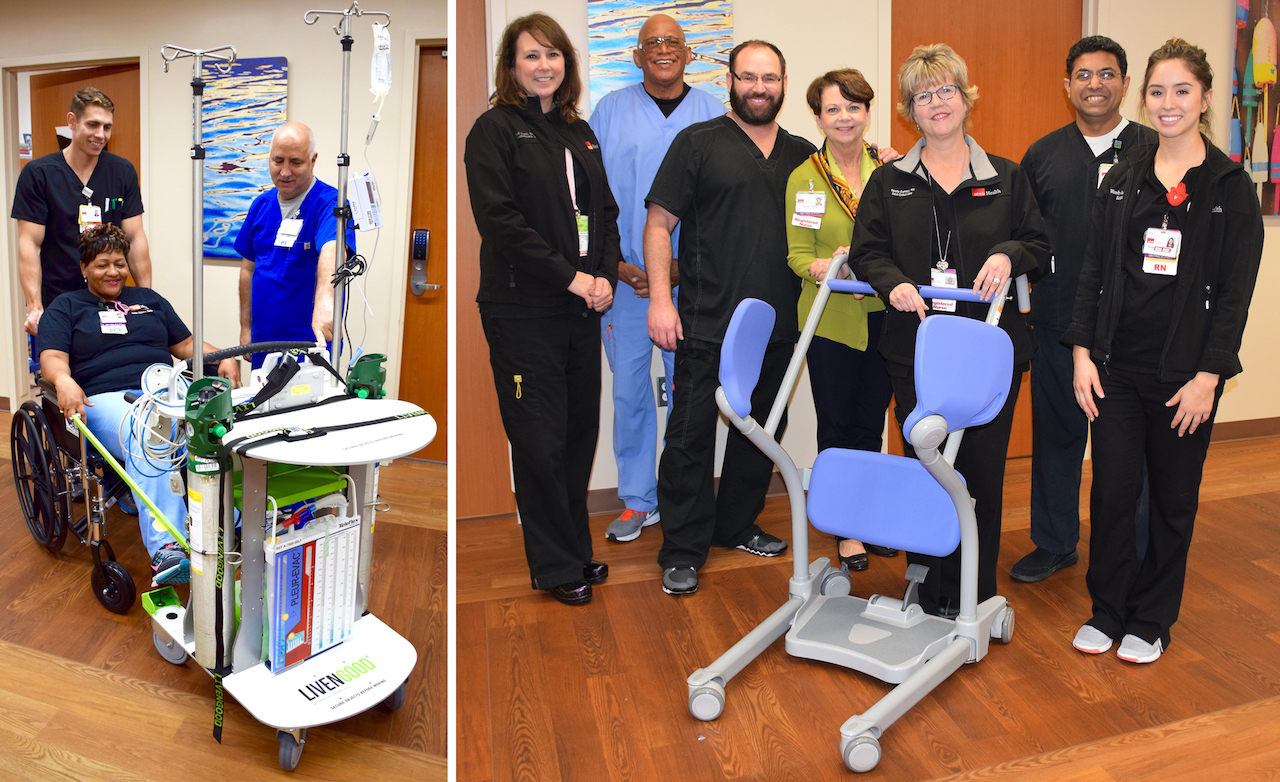
Mobility is a critical piece of patient recovery. Research shows the earlier a patient gets out of bed and starts moving, the better health outcomes they will experience. However, getting patients mobilized can pose a risk to health care personnel—lifting is dangerous and can lead to employee injuries.
A recent collaboration between UTMB Human Resources and Nursing Service is helping to solve that dilemma.
“Being a registered nurse is the fifth most dangerous job in America today,” said Kathleen O’Neill, UTMB’s director of Employee and Occupational Health. “People go into this profession to help—and end up as patients themselves. My goal is for every employee to go home the same way they came in.”
As an RN herself, O’Neill understands the relationship between patient mobility and health outcomes. Her office secured several grants and began working with Nursing Service a few years ago to bring assistive devices to UTMB, ultimately increasing patient mobility and independence while improving employee safety. After collecting data on employee injuries and patient needs, the decision was made to order several different types of equipment, including patient lifts and standing aids.
“These devices are a win-win for patients and employees,” said Odette Comeau, DNP, adult critical care clinical nurse specialist. “There’s plenty of literature out there to support the improved outcomes of patients who mobilize sooner. That includes things like shorter ICU and hospital stays and increased muscle strength. Along with that, employee safety is increased—when assistive devices are used, fewer staff are needed to mobilize patients, and those that are assisting are now freer from back injuries and other injuries.”
Dell Roach, nurse manager of the Surgical Intensive Care Unit/Intermediate Specialty Care Unit, added that the devices have changed the patient care culture at UTMB. Gone are the days of extended bed rest for critically ill patients. Now, nursing staff is committed to getting patients up and active as soon as possible.
“Staff has been amazed at how easy and simple the devices are,” said Roach. “They are now much more in the habit of reaching for the assistive devices instead of trying to move the patient without it.”
Most recently, a shipment containing 11 Livengood’s PACE devices arrived in March to be distributed to various hospital units, as well as UTMB-TDCJ Hospital Galveston. The device is basically a “souped-up” walker with shelves and hooks to hold all the patient’s equipment including ventilators, so all patients—even those in critical care—can take a stroll around the hospital.
“Now, patient equipment is clustered on one device, so they are holding on to it and moving with it and their tubes and lines are right there with them,” said Comeau. “This can help prevent inadvertent extubation, or pulling out tubes and lines, while still mobilizing the patient. And staff is excited. They liked piloting this piece of equipment so much, they kept asking when these would arrive. By providing them with a more hands-free approach to ambulating patients, we think it will result in fewer lost days due to injury and improve employee retention.”
Along with the new assistive devices, Nursing Service is taking a deeper dive into patient mobility. They recently formed a workgroup that meets weekly on mobility issues and has incorporated mobility protocols into onboarding training for new staff. In addition, Nursing has designated new mobility technicians to play a role on the overall health care team.
For O’Neill, this project has become her passion—and she’s already seen a positive impact.
“When we first got assistive devices in the Acute Care for the Elderly (ACE) unit, we were able to get a woman who had not been out of bed for two years into a wheelchair to eat and go outside for fresh air—that meant a lot to that patient and their family,” said O’Neill. “Her caregivers were not only taking great care of their patient, they were also protecting themselves from injury. I’d say that’s Best Care at its best.”