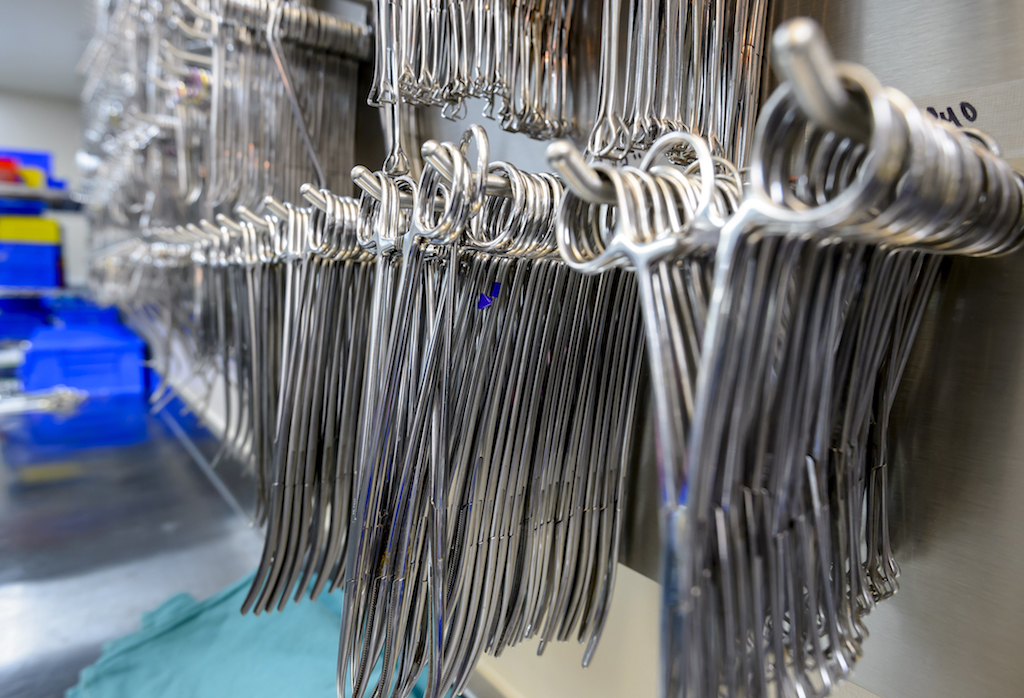

If you point at any one of the surgical instruments in UTMB’s Sterile Processing Department, bets are Lori Martin knows its name and purpose. No, she’s not a surgeon, but she plays a vital role in patient care.
As a sterile processing technician, Martin handles thousands of reusable surgical instruments and devices—from scalpel handles to fiber-optic endoscopes—every week. Her team runs a 24/7 operation and is responsible for washing, sterilizing, cooling, assembling, packaging and storing all medical devices and instruments used by UTMB, from Galveston to Huntsville.
“Making sure everything is clean, sterile and safe is work that is done behind the-scenes, but it feels good to know that we are protecting the welfare and safety of patients,” said Martin, who starts her day at 6:45 a.m.
I meet up with her on a Tuesday morning on the fourth floor of the Clinical Services Wing. After getting suited up in a protective hair net and white coverall that resembles an oversized bunny costume, I’m ready to enter the Sterile Processing Department.

“There are 70 surgeries scheduled today in the Jennie Sealy Hospital OR, so we’re busy getting instrument trays sterilized and prepped for the next procedure,” she says as she leads me into the decontamination room. The “decon” room is where carts holding dirty instrument trays come immediately following a surgery. It’s loud and lively, with techs taking apart, rinsing and soaking equipment before loading it onto industrial-sized automated washers. They look like my dishwasher at home on steroids—there’s even a giant washer for dirty carts. All employees wear protective gear, including face masks, gloves and gowns.
“We have to be careful to protect ourselves, too, from bioburden [bacteria living on a surface that has not been sterilized] and harsh cleaning chemicals,” says Martin. “Safety is a top priority in the decontamination room.”
Once dirty carts and instruments run through a wash cycle, they exit on the other side, which is sterile. Martin walks me out of the decon room and into the sterile room, where packing and sterilization begins.
Here, the washed instruments are sorted, inspected and counted at eight computerized workstations with bar code technology to track their location. Martin pulls up a “count sheet” at a computer workstation to assemble a retina instrument tray, used for eye surgeries.
“The count sheet tells us how many of each instrument is supposed to be in the tray,” she says. “Depending on the service, the trays contain different items. With this eye tray, you’ll notice all the instruments are much smaller than a tray for an orthopedic surgery, for example.”
Martin picks up the completed tray and wraps it in a blue medical grade paper that acts as a barrier to air and waterborne contamination. She adds a piece of tape to the outside of the package before adding it to a load that is ready to go into an autoclave.
“The tape plays an important role,” says Martin. “It changes color from white to black to indicate that the sterilization cycle ran at the proper temperature for the right amount of time. To be properly sterilized, temperatures have to reach at least 270 degrees Fahrenheit. We also include a biological indicator [BI] in each load. It uses microbes that are highly resistant to sterilization. When the highly resistant bugs contained inside the BI are killed during sterilization, we can be confident that all the instruments are sterile and safe.”
While Martin helps out in all areas of the department, she can usually be found in the

stock area, among seemingly endless aisles of sterilized trays that are ready for use. She sorts and restocks trays according to their service, such as cardiovascular or urology.
She introduces me to Raoul Simmons, a sterile processing tech who helped train Martin when she started four years ago. The two have forged a great working relationship and are known for teaming up to get the job done fast and efficiently.
“When things get chaotic, we don’t even have to talk to each other; we just know how the other person operates and what needs to get done,” said Martin. “I really like the people I work with. Everyone is great and has a wealth of knowledge. If you need anything, they are there for you.”
Just as she finishes that thought, the phone starts ringing and the pace picks up. A nurse is on the line, and she needs a specific instrument delivered to the OR quickly, as the surgeon is in the midst of a pediatric surgery.
“Want to see the OR?” Martin asks as she heads for the door. As we walk briskly toward the Jennie Sealy Hospital OR, she tells me she can take about 20,000 steps a day, delivering items to the OR at a moment’s notice.
“If the surgeon wants a certain item that isn’t on the original case cart or if an instrument gets contaminated, we have to replace it quickly,” said Martin. “If we don’t have a particular instrument, we may have to take it off of another case cart and give it to the surgery that is happening right now and then turn it over quickly so it’s ready to be used again a few hours later. I try to keep everyone happy and make sure they have all the instruments they need.”

We enter the centerwell area, which is in the middle of all the operating rooms and holds supplies and instruments that can be grabbed quickly during surgery. Martin knocks on the door of one of the ORs and hands the tray over to a nurse, who is grateful for the fast service.
I say goodbye to Martin as she heads back to prep case carts for the next day’s surgeries. She sorts out preference cards for each case, which includes the surgeon’s name, instruments requested, procedure, location and other information.
Martin may not have direct contact with patients, but she is truly one of the unsung heroes of patient care. Her attention to detail and commitment to best care is evident in all she does.
“Every day, people come to UTMB for life-changing surgeries,” she says. “I’m proud to be a part of the overall mission and, ultimately, help deliver positive patient outcomes.”