Tim Robinson’s attention to detail is one of the most important traits he acquired in the Navy—and one that has helped him throughout his career.
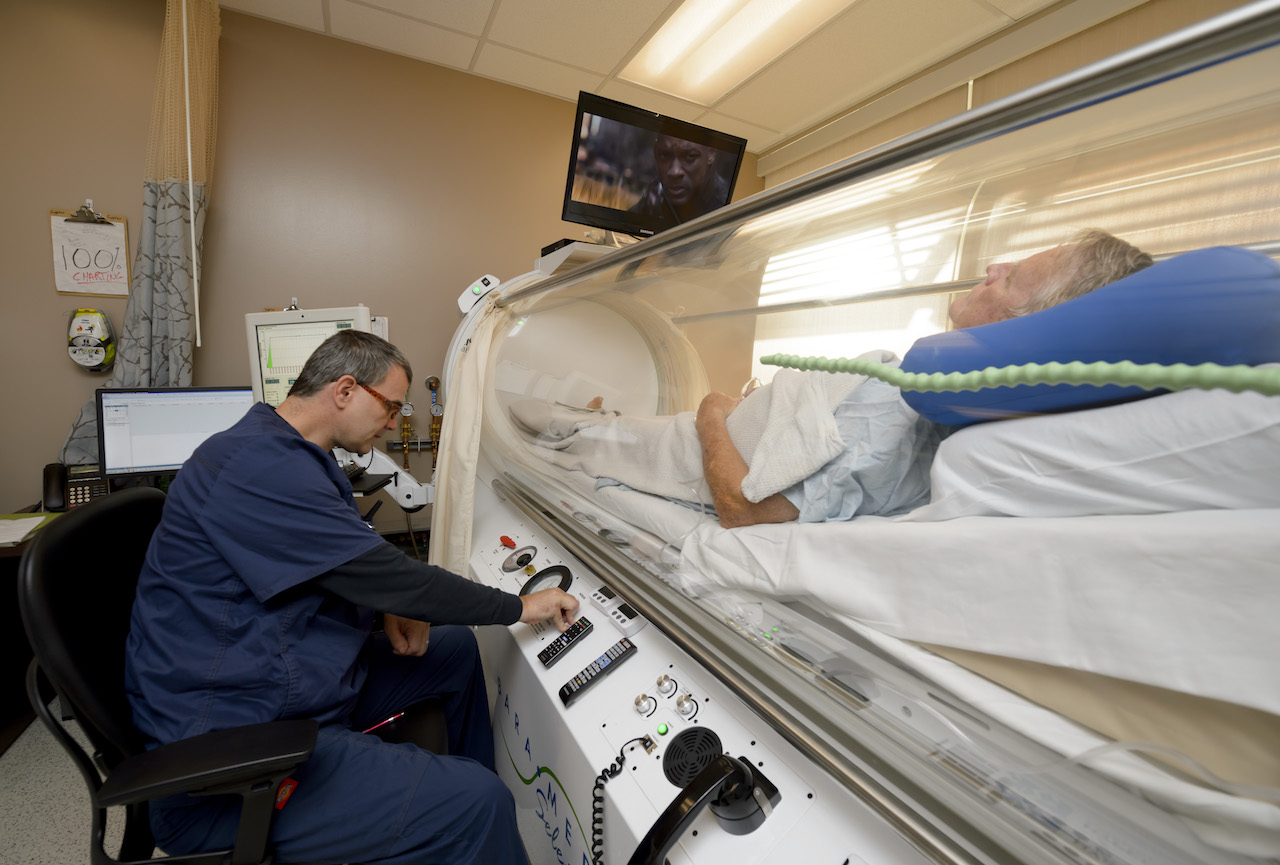
His military state of mind is evident the moment I meet him at UTMB’s Wound Care and Hyperbarics Clinic in Dickinson. Opened in late April, the clinic provides specialized wound care treatment and hyperbaric oxygen therapy (HBOT) to heal serious infections and chronic wounds. HBOT takes place within a total body chamber, where breathing 100 percent oxygen under increased atmospheric pressure enhances the body’s natural healing process.
As a certified hyperbaric technician, Robinson is the first to arrive at the clinic at 7 a.m., making turbo-strength coffee and going through a series of checklists prepping for the first patients.

“There’s a certain discipline you must have in my position. Things must be done a certain way, at a certain time, in a certain order,” says Robinson as he grabs a clipboard and begins checking the air, oxygen and oxygen back-up systems. “I literally have checklists to make sure I do my checklists. We follow demanding safety protocols—safety is our No. 1 priority.”
Robinson’s path to becoming a hyperbaric technician started at age 17 when he graduated from high school and went directly into the Navy. He spent four years as a weapons specialist and corpsman before attending college and qualifying as an underwater welder and a certified hyperbaric technician and diving medical technician.
Robinson says many who follow this path into medicine have a commercial or military diving background, while others simply want to learn about the mystique of hyperbarics.
“It’s not voodoo medicine—it’s simple physics and physiology perfectly mixed into a recipe of healing,” says Robinson. “Almost every process in the body is oxygen-dependent in one way or another—from basic respiration to our ability to fight infection. With hyperbarics, every treatment saturates the body with pure oxygen [the oxygen concentration in air is 21 percent] at greater atmospheric pressure [similar to a SCUBA diving session]. The treatment helps push more oxygen further into the tissues, ultimately speeding the healing process.”
While HBOT is known for treating diving-related injuries such as decompression sickness (“the bends”), Robinson says it’s also proven to help heal more than a dozen types of serious infections and chronic wounds, when used in combination with other treatments. The most common he sees are wounds caused by diabetes, poor circulation and bone infections.
As Robinson shows me the two “monoplace” chambers, which can accommodate

one patient at a time, a nurse practitioner comes in to tell us the first patient has arrived. We walk to the front of the clinic and Robinson greets the patient, who has been coming for treatment five times a week for the past month. The two pick up conversation where they left off the day before. Today’s discussion centers around the recent Astros win and a story about the patient’s time as a former bomber pilot in the U.S. Air Force.
“I love the patient interaction aspect of my job,” says Robinson. “Standard procedure for wound healing is one ‘dive’ per day, five days per week for a total of 20 to 30 treatments. So I am with patients for months on a daily basis. I know about their cat, who won the baseball game in the Pee Wee League and what the grandkids are doing.”
Once vital signs are taken and a physician stops by, Robinson makes sure patients are comfortable before carefully pushing them into the chamber. He loads a movie on a DVD player to keep patients occupied during the 110-minute treatment.
“Mark time 08:30, leaving surface, Chamber Two,” says Robinson into a two-way radio. “Each dive is usually just under two hours. We start with a 10-minute descent to compress the patient to ‘depth’ and finish with a 10-minute ascent. We call it a 110-minute profile.”
Robinson sits next to the chamber the entire time, evaluating the patient, taking detailed notes and ensuring the chamber is running properly. He stays in close communication with clinic staff throughout the dive, who are trained to handle the chamber in emergency situations.

“The people I work with every day are fantastic,” says Robinson. “We’re a multidisciplinary team of certified hyperbaric technicians, nurses, nurse practitioners, a physician assistant and physician specialists—including a podiatrist, dermatologist and vascular and plastic surgeons—who closely collaborate with infectious disease and orthopedic physicians, and occupational and physical therapists. The wound care we provide is an important adjunct to surgical care also offered.”
Once the dive is finished, the patient tells me how impressed he’s been with the staff and the results of hyperbaric treatment. After battling a chronic venous ulcer on his ankle for more than two years, he’s finally noticed that the wound has been healing—and he hopes to one day be able to go swimming in the ocean again.
Robinson’s day includes one other hyperbaric patient who developed a bone infection following open heart surgery. He’s quick to remind me that HBOT alone is not enough to mend non-healing wounds.
“Hyperbarics is meant to be used in addition to other therapies,” he says. “So patients are also getting compression bandage changes, dressing changes, taking medications, etc., and we are a secondary, or adjunct therapy. We always encourage our patients to continue interacting with their physicians, taking their medications and letting us be part of their team to help them with their overall healing.”
After treating the two patients with HBOT, Robinson’s afternoon consists of wound care consults and dressing changes. I watch as he saws off a fiberglass cast designed to take weight off the foot in patients with diabetic foot ulcers. The patient comes in weekly for cast changes and Robinson takes pictures and measurements of the wound at each visit to document progress.
“We submit the photos and detailed documentation directly to the patient’s physician

so they know everything we did and can make recommendations for next steps,” says Robinson. “Everything we do has specific physician orders—we don’t improvise or do anything without talking to them first.”
Robinson says some UTMB physicians have already been referring patients to the wound clinic, and he hopes to continue building those relationships, along with the clinic’s patient load—because it’s that military mindset of attention to detail and genuine care for each individual that saves limbs and lives.
“If a wound doesn’t heal, some patients could lose their limbs—and that could end with poor results if they have difficulty adapting to their new situation,” says Robinson. “We give them the chance to avoid that. I get to see a wound from beginning to end and not many other clinics can say that. A lot of these patients have had wounds for years—not days or months. For them to come to our clinic and see their wound heal—it’s a relief for them and it’s great for us to see.”