

Every day, Jeanene Trochesset sees how organ donation and transplant medicine provide recipients with a second chance at life.
She’s spent the last 31 years working in nephrology-based positions at UTMB—from a pediatric dialysis nurse, to her current role as a post-transplant coordinator for UTMB’s kidney and pancreas transplant programs. A certified nephrology nurse, Trochesset provides clinical management of hundreds of transplant patients from Lafayette, Louisiana to McAllen, Texas and helps them adjust to their new life after transplantation.
“It’s always exciting to see our patients thrive after a transplant and experience a better quality of life free from dialysis,” says Trochesset as I meet up with her on a Monday morning. “We have an entire team that cares for patients from the moment they are referred to us until after they are transplanted—and beyond. The team consists of intake coordinators, pre- and post-transplant coordinators, a waitlist coordinator, assistant coordinators, social workers, dieticians, transplant surgeons and a transplant nephrologist.”
She’s getting ready to start a half-day post-transplant kidney clinic, which is held twice a week at the Multispecialty Center and Stark Diabetes Clinic in League City. There are more than a dozen patients scheduled for post-transplant appointments—all before noon.
“This is a really busy clinic—it goes really fast and furious from when we start the clinic to when it ends. Coffee anyone?” she laughs and greets her colleagues, which include another post-transplant coordinator, waitlist coordinator, physician and nutritionist.
 Trochesset with team members (L-R) Brenda Rush, Dr. Muhammad Mujtaba, Trochesset and Janice Parson.
Trochesset with team members (L-R) Brenda Rush, Dr. Muhammad Mujtaba, Trochesset and Janice Parson.They all sit in the “team room,” a small area in the middle of the clinic with computers lining the walls. Before clinic doors open at 8 a.m. is the only time the team will be seen together in one place—once things get started, Trochesset and her team quickly disperse into patient rooms, passing each other in the hall throughout the day.
“We usually have one of our transplant surgeons here during the clinic, as well, but Dr. Kristene Gugliuzza just finished a kidney and pancreas transplant this morning in Galveston,” Trochesset says. “Donor organs can become available at any time, so the team is always ready. The amount of transplants UTMB performs has really ramped up the last few years.”
In fact, last December saw the highest number of kidney transplants within a month in the program’s 50-year history—14 transplants. Since 2014, the kidney transplant team has increased the transplant volume by 156 percent.
UTMB has been a pioneering force in transplantation since 1967, when the first kidney transplant in Texas was performed on the Galveston Campus. UTMB performed its first liver transplant in 1992, followed closely by heart transplant in 1993. Through a grant from The Sealy and Smith Foundation in 2007, UTMB established the Texas Transplant Center. Today, the center offers heart, liver, kidney and pancreas transplant services to the greater Texas Gulf Coast and has completed more than 3,200 transplants to date.
Trochesset introduces me to her counterpart, Janice Parson. Together, the two women, along with the help of four assistant coordinators and a part-time coordinator, monitor more than 800 kidney and pancreas post-transplant patients.
“Once we have a patient, we have them for life,” says Trochesset. “We really get to
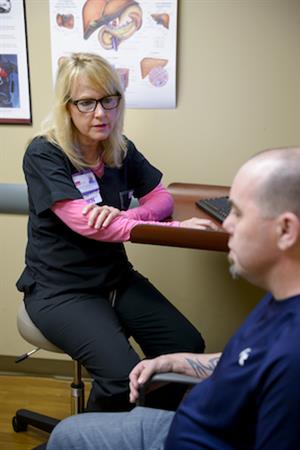
know each patient and their family. Taking prescribed medications, keeping up with lab work and regular clinic appointments are key to keeping their kidney safe. Each patient is different. I know patients who have had three kidney transplants—and then I also know lots of other patients who have had only one transplant that lasted for 20-plus years and their transplant is still working fine.”
Many patients get labs before arriving at the clinic to be seen by one of the post-transplant coordinators and physicians. Typically, Trochesset sees patients twice a week for the first month following their transplant, then every two weeks, once a month, every three months, and so on. Two years out, she may see patients every six months to a year. It all depends on how smoothly the transplant surgery went and if there are any signs of organ rejection.
“We have two sets of patients,” says Trochesset. “The immediate post-op patients who have just received their transplant and need their surgical wound to be observed by the surgeon, and then the patients who are all healed and may have received their transplant several years ago who will see the transplant nephrologist. In my role, I usually talk to the patient first and give the doctor a heads up if anything urgent needs to be addressed.”
Her first patient of the day arrives carrying a large bag full of various medications, supplements and anti-rejection drugs. He had a kidney and pancreas transplant two years ago and will be on two anti-rejection drugs and other medications for the rest of his life.
“A transplant is not a cure, it’s a treatment,” says Trochesset. “The same thing that may have caused a kidney to fail the first time can cause it to fail again. If a recipient has diabetes, heart disease or other comorbidities—and they do not keep all of them in control—the comorbidities could cause problems with their transplanted kidney. As a result, I spend a lot of time educating patients about staying healthy and taking prescribed medications.”
So far, the patient seems to be doing well post-transplant, and has gone back to work full-time. Trochesset knows the patient well—she spends time asking about his family and how he has been feeling since she saw him last. When she finishes checking out his medications and refills, the nephrology physician pops in to complete his assessment, review lab results and ask a few more questions before scheduling the next appointment for six months later.
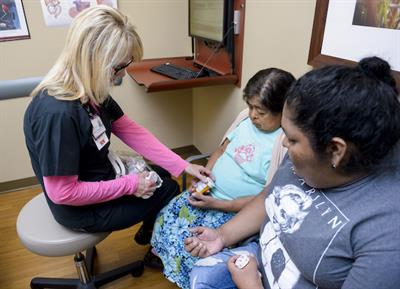
I start noticing a pattern as each subsequent patient arrives holding a large bag of medications.
“That’s one of the big things—making sure patients have all their medications, are taking them when they are supposed to in the correct doses, and are not out of anything,” says Trochesset. “We literally go through each patient’s medications one-by- one and check it with our list. There are a lot of medications and it can be really intimidating, so I do everything I can to help patients become familiar with them so it’s not as daunting.”
One of her patients received a kidney three weeks prior. It’s the woman’s second kidney— and Trochesset had the honor of informing the patient that a kidney had been donated and was available.
“I was on-call that night and got to call her in for the transplant,” Trochesset says with tears forming in her eyes. “To tell you the truth, I still get choked up sometimes— it’s such a special, critical moment. Patients are like, ‘Are you kidding me?!’ They are always so excited and grateful.”
Currently, there are more than 350 people on UTMB’s kidney waitlist and 90,000

nationwide listed for kidney transplant. It can take days, months or many years before a compatible match is found; however, Trochesset points out the process of living donation can cut down wait time and improve the likelihood of the transplant lasting longer. A person can live and function normally with only one kidney, so it’s not uncommon for relatives, friends and others to serve as living kidney donors.
Trochesset heads to the team room to get a quick sip of coffee and take a look at the white board listing all the patients who have arrived. The list gets longer and longer throughout the morning, and Trochesset goes from one room directly to the next.
One of her last patients of the day had a transplant the previous month and Trochesset immediately suspects he is having complications. In addition to a small infection at the surgical site, his symptoms and lab results point to signs of organ transplant rejection. She changes the wound dressing and discusses her findings with the nephrologist, who comes in to assess the patient for possible changes to the plan of care.

“When we look at lab results, the first thing we look at is the creatinine levels because that tells us the patient’s kidney function,” says Trochesset. “Next, we check other labs such as their tacrolimus (an immunosuppressant used to prevent transplant rejection) levels and urine analysis for any abnormalities. Any abnormal labs may signify a possible adverse event or rejection. I’m a stickler for detail, so I always review the patient’s labs with them and make sure they understand what they need to do.”
The doctor asks Trochesset to order a biopsy for the patient and medication to help lower his potassium levels, which is critical to the function of nerve and muscle cells.
“The patient has to take this medication today because high potassium levels can be very dangerous,” said Trochesset. “If I order it from a pharmacy and they don’t have it, I have to call around until I find it—I don’t want anything to fall through the cracks. We try really hard to take special care of our patients and if they do have a problem, like they need a biopsy, it gets first priority. There are ways to treat transplant rejection, but we have to act quickly.”
It’s 1 p.m. by the time Trochesset finishes up with the last patient and gets ready to

drive back to the Rebecca Sealy building on the Galveston Campus, where transplant offices are located. I learn she was born in Rebecca Sealy—then St. Mary’s Hospital—just a floor below her current office.
She’ll spend the rest of her day prepping for her next trip to McAllen (she sees post-transplant patients there about once a month) and answering patient emails and calls.
As we part ways, I reflect on how organ transplant saves many lives each year. However, the procedure is only the beginning of a new life journey for the recipient—a journey that Trochesset is proud to be part of.
“I really enjoy helping these patients get that second chance,” says Trochesset. “It’s not just my job, it’s my passion.”