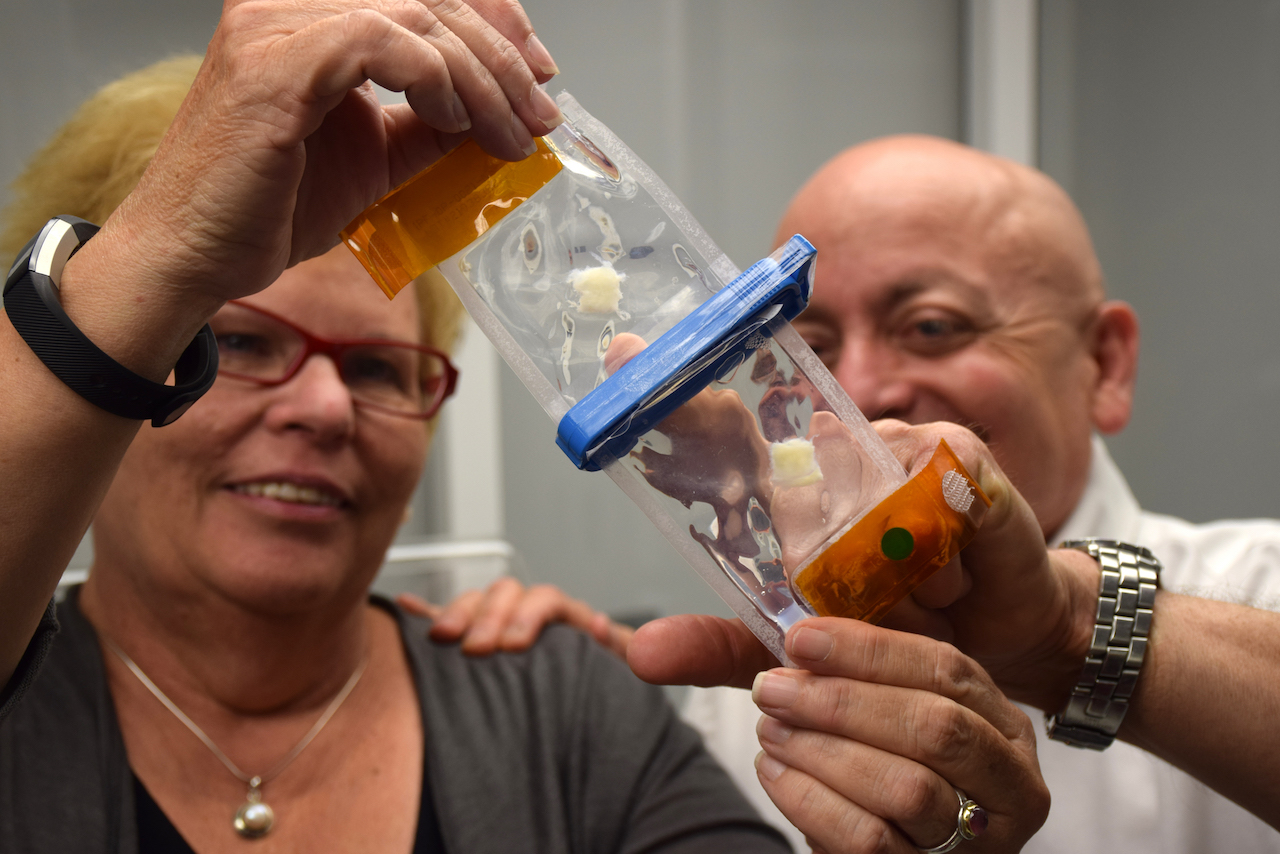
Growing up during an era with an active space program, Dr. Joan Nichols and Dr. Joaquin Cortiella were fascinated by space.
Nichols, professor of Internal Medicine and Microbiology and Immunology and associate director of research and operations for the Galveston National Laboratory at UTMB, vividly remembers learning about each of the Apollo missions and astronauts like John Glenn.
Now, she and Cortiella, a professor and physician in the Department of Anesthesiology at UTMB, are having the chance to live a childhood dream.
“Who on Earth would have thought that two kids from New York would someday send something into space?” Cortiella said. “For us, this was a dream come true.”
In August, Nichols, Cortiella and members from their lab traveled to Cape Canaveral, Florida, for the launch of an unmanned SpaceX resupply mission to the International Space Station. On board the SpaceX rocket were some of the UTMB lab’s lung cell samples that astronauts would grow, hopefully allowing researchers to see the implications of spaceflight on the lungs of astronauts, as well as those of us still on Earth. The research could possibly lead to future therapeutics for various lung diseases.
But getting the samples into space wasn’t that simple. The mathematics and science behind making that possible is truly phenomenal, Nichols said. It took years of planning and working with NASA and others to make sure the experiment would work safely in space.
What went up were lightweight bioreactor pouches containing lung progenitor cells and stem cells, as well as pieces of lung scaffolding. Progenitor cells are a type of stem cell that are usually limited to maturing into one, or very few, cell types. Other stem cells can develop into any kind of cell. The scaffolding is a collagen and elastin frame on which the lung cells grow.
Each of the bioreactor pouches were adapted so that the experiments could be done in microgravity. Scientists from UTMB and Houston Methodist Research Institute worked closely with NASA to come up with an understanding of how to take their model and adapt it to a low-gravity environment.
“We didn’t know how to approach space flight at all,” Nichols said. “We are used to growing our samples in small culture dishes or bioreactors, which are like bottles but big and heavy. Going into space, things have to be very light because the heavier it is, the more expensive it is to send.”
The bioreactor pouch design helped shed the necessary weight. Other adaptations included attaching Velcro to each of the pouch’s caps so they could be tethered and not get lost in the zero gravity environment. Nichols and Cortiella also developed precise, simply worded instructions so the astronauts could manage and run the different experiments on the samples.
“I spent weeks writing out the procedures,” Nichols said. “We have written—I don’t know how many—two-sentence blurbs, five-sentence blurbs for astronauts to understand.”
Once the materials were ready, it was time to turn their attention to the actual trip to the space station.
“Our hearts were pounding. It’s like you’re in awe and don’t believe it until it actually happens,” Nichols said. “We were wondering, ‘Is it going to take off? Is it going to make it to orbit? Once it gets into orbit, is it going to dock?”
Once they received confirmation the rocket had successfully launched, everyone was in tears and jumping around, Nichols said.
“People in the stands realized who we were because we all had on our ‘Lungs in Space’ shirts on,” she said. “People saw we were there and began applauding us and asking us about the project.”
Researchers have already learned a lot about how long-term space flight can affect a person’s eyes, bones, muscles and heart. But now with NASA’s sights set on traveling to Mars, UTMB scientists think it’s important to think about other tissues, such as the lungs, and what their responses might be–or how the lungs might be altered by space flight.
Now that the lungs have returned to Earth, researchers will evaluate how the cells have changed in space, including structure of the tissues, response of immune cells and whether the cells developed fibrous tissue in response to damage, or fibrosis. Previously, lung injuries have been found to accelerate in space, and close study of these cells may help in developing therapeutics.
“We know that there are some problems with lungs in space flight, but that hasn’t really been closely looked into,” Nichols said. “We hope to find out how lung cells react to the change in gravity and the extreme space environment, and then that can help us protect astronauts in space, as well as the lungs of regular people here on Earth.”