
When a patient arrives at the emergency department on UTMB's Galveston Campus, there’s a good chance Vonday Millier will be the first university employee they see.
“We really set the tone for the patient’s visit,” says Millier, a patient registration specialist and team leader within Revenue Cycle Operations (RCO).
Hearing the words “revenue cycle” might lead a person to believe Millier sits behind a desk all day, crunching numbers. However, for the past 15 years, she’s been in the ED working alongside patients, nurses and physicians to provide excellent customer service and ensure the overall success of UTMB’s clinical enterprise.

Patient registration is the first step of the revenue cycle process—which begins when a patient is identified as needing or requesting medical services, and ends at the time payment is received and the account is closed. Getting accurate information from the start—such as patient identification, and demographic and insurance information—is a crucial part of the process that not only affects billing, but even more importantly, patient safety. Every piece of data collected by the registrar is used by other hospital staff, clinical and non-clinical throughout the patient’s stay.
I got a firsthand look at how the registration process works shortly after meeting up with Millier on a Monday morning in the ED. As she reviews the day’s staffing schedule, a pager nearby starts to beep, signaling the arrival of an ambulance. She quickly makes her way to the ambulance bay in the back of the department as two emergency medical technicians push a stretcher through the doors.
“Hello, my name is Vonday and I will be registering you this morning,” she says to the elderly patient who seems confused after falling and hitting her head. “Can you tell me your full name and date of birth?”
The woman has trouble remembering her name, so Millier speaks with the patient’s husband to verify her identification and sign a “consent to treat” form. At the same time, a nurse starts taking the woman’s blood pressure and asking his own set of questions.
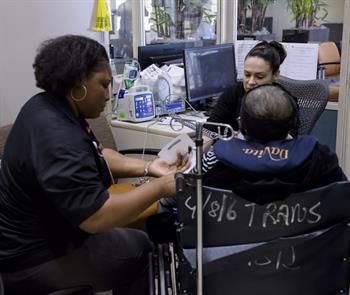
“We call it ‘tag teaming,’” says Millier. “While I’m asking the patient their name and date of birth, the nurse is also asking them what brings them to the ED and taking their vitals. We work closely with the nursing staff—it’s a good relationship.”
This isn’t the first time the woman has received care at UTMB, so Millier is able to search UTMB’s Epic electronic medical record (EMR) for the patient’s existing medical record number. She’s careful to double-check the woman’s information in the system before pressing the ‘arrive’ button.
“By hitting ‘arrive’ in the system, I’m basically checking the patient in,” says Millier as she places a bar-coded I.D. armband around the patient’s wrist and prints additional patient labels to give to the nurse.
The bar-code technology is used to promote patient safety and reduce medical errors. Not only does the wristband identify the patient, it also connects the patient to their existing electronic medical information. In addition, when medication needs to be administered, a quick scan of both the wristband bar code and bar-code label on the medication will immediately verify prescription and treatment information. Millier says it’s important for the initial registration to be done quickly and accurately so the patient can begin receiving care.
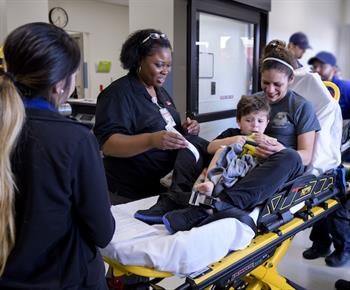
“Now, the nurse can take the patient to a room and the physician can access the patient’s existing medical history if it’s in Epic and start documenting the care in the EMR,” she says. “The initial registration takes just one or two minutes, but I’ll be back to interview the patient once they’ve been seen by a doctor. ED patients already are not feeling well, so they appreciate having registration completed at the bedside where they’re more comfortable.”
The Galveston Campus ED is one of the busiest areas of the hospital; an estimated 45,000 patients are expected to go through it this year—and each and every one of them will be seen first by a registration specialist. It’s a 24/7 role, with about five registrars and a team leader working at any given time to cover the triage, ambulance bay, inpatient and minor emergency treatment areas.
“No day is the same here—it’s an adrenaline rush for sure,” says Millier. “Not everyone can adjust to seeing sickness and trauma all the time, so it takes a strong-minded person who is also compassionate and empathetic to have this role. Oftentimes, we handout blankets, comfort families or just sit with the patient and listen to them vent. We meet people from all walks of life.”

Over the next few hours, Millier registers several more patients, creates medical record numbers for those who are new to UTMB, helps troubleshoot a computer issue and completes a deposit of patient cash payments from the overnight shift. By noon, the pace has picked up and the number of patients in the ED has gone from 15 to nearly 40.
She turns her attention to bedside interviews, as several patients have been seen by a physician and are either ready to be discharged or admitted to a hospital unit. She allots about 30 minutes per patient, verifying additional information such as the patient’s mailing address, religious preference, employer and insurance.
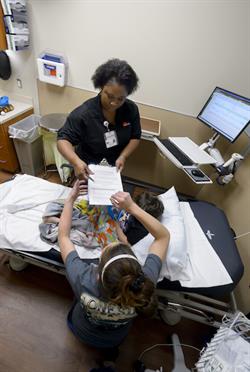
“We don’t ask them about insurance information until we get to the bedside,” says Millier. “But even then, you have to read the situation and sort of ‘break the ice’ before launching into the interview. Many times, people are still processing whatever information their doctor just told them, so it’s important to be mindful of that. I make sure to scan the room and ask everyone what their relationship is to the patient. If the patient is not feeling well or is unable to speak, I will ask for permission to talk to their relative.”
One of the rooms she enters has a young boy and several family members. Fortunately, everyone seems to be in good spirits, as the boy has recovered from a severe asthma attack—he’s even bouncing up and down on the bed, ready to go home. Millier compliments the child for being so brave while quickly verifying insurance information, collecting a co-pay and providing a receipt to his mother.
“We have to be knowledgeable about all types of commercial and government health insurance plans and if there are multiple insurance policies, how to prioritize them for billing,” she says. “We try to collect payments while patients are in the ED and answer any questions they may have about their financial responsibility. It can be confusing, but we are here to help.”
Oftentimes, the bedside interview is an opportunity for Millier and her team to discuss resources available for uninsured or underinsured patients.

“There are many resources, but we find that a lot of people are unaware of them,” she says. “Sometimes, we can really help just by giving a patient a financial screening packet for a discount or giving them information for applying for Medicaid. I can also enlist the help of a social worker if the patient needs additional services.”
After working for more than a decade in the ED, Millier isn’t immune to noticing all the trauma, but she takes it in stride. She often finds herself driving home, thinking about patients and brainstorming additional resources that could benefit them.
“We try to help everyone,” she says as she heads to the triage area.
A late-afternoon wave of walk-in patients has arrived and Miller will be the first to greet them—doing what she can to help each patient navigate their way to better health.