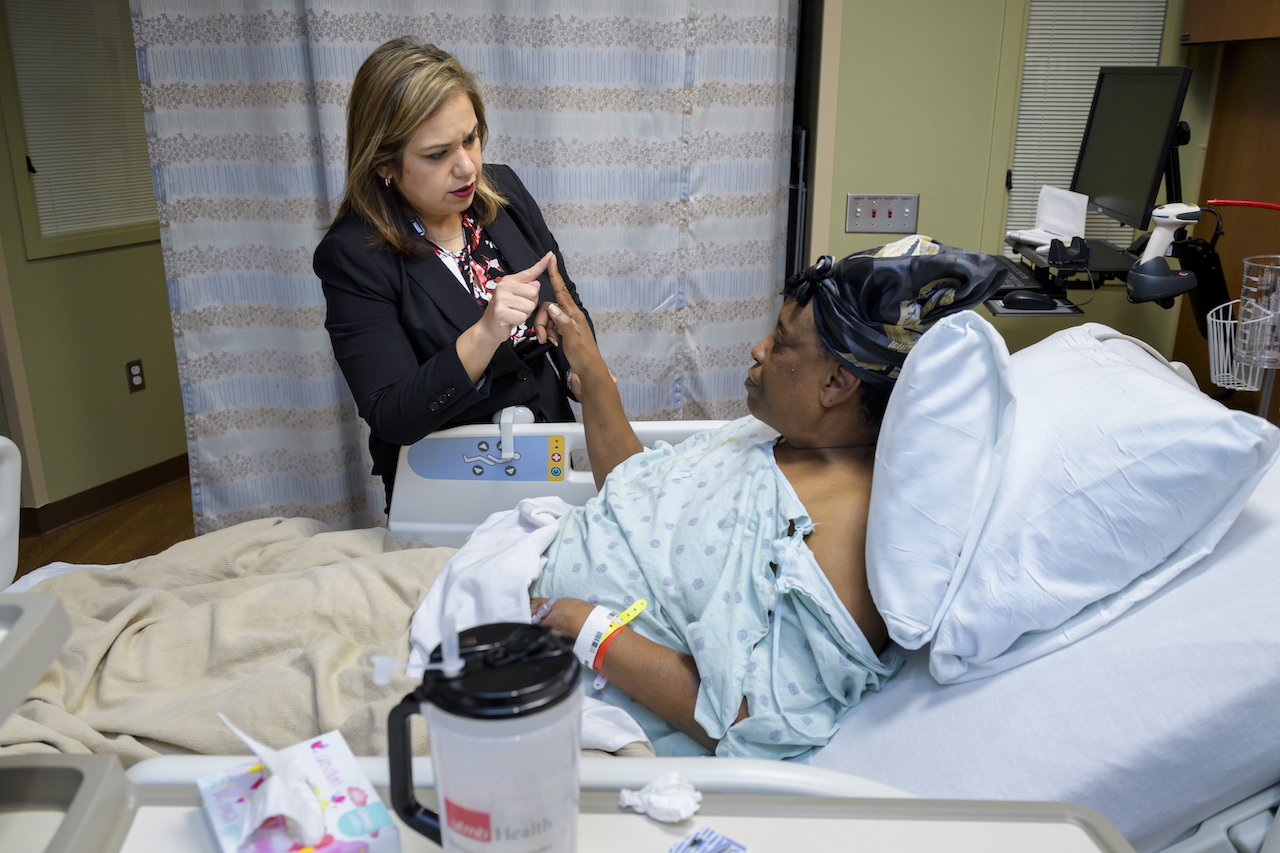

UTMB Stroke Coordinator Brenda Yanez lives and breathes the mantra “Time is brain.”
“Every minute counts after a person has a stroke,” she says. “About two million brain cells die each minute during a stroke, so knowing the symptoms and getting help quickly is key to reducing or even reversing the effects.”
Stroke—which occurs when a vessel in the brain ruptures or is blocked by a blood clot—is a leading cause of death and long-term disability in the U.S. For the past three years, Yanez has been on a mission to change that. As stroke coordinator for all UTMB campuses, she is leading the charge to continuously improve stroke services and spread awareness about the risk factors and signs of stroke to medical staff, emergency medical services personnel, patients and families.
I meet up with Yanez on a Thursday morning, as she heads to daily interdisciplinary rounds on the neurology and neuro critical care units in Jennie Sealy Hospital on the Galveston Campus. At any one time, Yanez tracks about 10 to 15 stroke patients across the hospital. The rounds serve as an opportunity for collaboration among all care providers, including nursing staff, care managers, dieticians, pharmacists, residents, physical therapists and others.

“We discuss each stroke patient and their plans for treatment, discharge and rehabilitation,” says Yanez, who previously worked as a nurse in the Galveston Campus Emergency Department. “UTMB has been certified as a Primary Stroke Program by The Joint Commission since 2013. We are currently working toward Comprehensive certification because we can handle the most complex stroke cases—including going into the brain and mechanically extracting blood clots. It’s exciting because most places can’t do that.”
Yanez listens as the care team discusses stroke patients of all ages—including one man in his 30s who has a hole in his heart, which likely was a contributing factor.
“There’s a misconception that only the elderly can have strokes, but it can happen to anyone,” she says. “A clot from somewhere in this patient’s body may have traveled through the hole in his heart and blocked an artery in the brain. We will be consulting with cardiology to see if there are treatment options to close the hole and help prevent future strokes.”
As the meeting ends, Dr. Adham Kamel, stroke medical director and

assistant professor in the Department of Neurology, arrives with a team of residents. Yanez accompanies Kamel as he makes his rounds, checking in with each patient and their family to make sure each they understand the plan of care.
Yanez is happy to see how well one woman is doing the day after having a stroke. Luckily, the woman was brought in to the hospital quickly after symptoms of slurred speech and dizziness began. The stroke team was able to give the patient tPA, an intravenous drug that dissolves clots.
“tPA needs to be administered within four-and-a-half hours of the onset of stroke symptoms,” she says. “When I saw her yesterday, she couldn’t move one whole side of her body, but today, you can see huge improvement. It’s amazing—she can move both sides of her body and is already getting back to normal. tPA can be life-changing and live-saving when patients get to the ER quickly.”
Yanez does some coordination exercises with the woman, asking her to touch her pointer fingers together and then touch her nose. The patient has a hard time at first, but repeats the exercise until she can do it almost perfectly.
“Don’t get frustrated with yourself, you are doing very well,” Yanez says encouragingly. “Now it’s time to get up and start moving. Physical therapy is going to come by today and get you out of the bed and into the chair. If you don’t use it, you’ll lose it!”
She reassures the patient and her husband that she will be back later to check on them. In the meantime, Yanez and Kamel visit another patient who had a transient ischemic attack, or TIA. Known as a “mini-stroke,” it is a temporary blockage of blood flow to the brain and can indicate the likelihood of a coming stroke.
Yanez takes the opportunity to educate the patient about stroke symptoms

such as face drooping, arm weakness and speech difficulty. She also stresses the importance of calling 911 immediately, as the patient waited several hours before calling his daughter for help.
“The most important thing is making sure you come straight to the ER next time because the longer you wait, the more irreversible damage is done,” she tells the patient. “And once you have one stroke, you are at a higher risk of having another one. If you were having chest pain, you would call 911 right away, right?” The patient nods. “I know you worry about your heart, but your brain is important, too—it makes your heart function.”
Patients seem to appreciate Yanez’s kind but straightforward demeanor. She speaks from the heart, as her own mother suffered a stroke less than a year ago. Fortunately, her mother was able to get tPA at UTMB and has made a full recovery, but Yanez knows not everyone has a positive outcome.
“The biggest challenge is public awareness,” she says. “How do we get people to recognize when they are having a stroke and call 911? Or how can they prevent a stroke in the first place by making lifestyle changes such as quitting smoking or lowering blood pressure? A lot of times, people get symptoms in the evening and try to sleep it off or they’ll wait and try to set up an appointment with their primary care provider. But, by the morning, it’s too late.”

Yanez’s passion for educating patients and health care staff shows in everything she does. In fact, if she hadn’t become a nurse, she wanted to be a teacher. Now she gets the best of both worlds. After finishing up rounds with Kamel, she heads to the Rebecca Sealy building to teach new nursing hires about UTMB’s stroke program. She spends about 20 minutes during their orientation going over stroke risk factors, stopping to answer questions and offering herself as a resource in the future.
“I encourage you to educate your patients on risk factors and stroke prevention,” she tells the class. “Even if your patient isn’t having a stroke when they come through the door, they may be hypertensive and diabetic—that combination dramatically increases their risk for stroke.”
In addition to teaching during nursing orientation, Yanez is proud to offer eight-hour-long advanced stroke life support classes to nurses across UTMB. So far, she has helped train about 200 nurses and is recruiting “stroke champions” to continue spreading awareness in their units.
By the afternoon, Yanez gets ready to head back to her office to analyze

stroke readmission data and make follow-up calls to patients who were recently discharged. But before she gets there, her cell phone beeps, signaling a “stroke activation,” which is called when a patient is identified as having stroke symptoms that began within the last six hours.
A patient has just arrived to the ED with facial paralysis and blurred vision, so Yanez immediately heads over to try and help the ED nurses, physicians and residents. When she gets there, the patient has already been wheeled to radiology for a head CT scan. If the scan comes back clear of any bleeding, the patient may be eligible to move forward with tPA or intra-arterial treatment, which removes blood clots by advancing a catheter through an artery in the groin, up to the site of the clot.
“It is a symphony of people—from EMS to the ED nurses and doctors, neurologists, CT and lab personnel—working together as a team to diagnose and start treating stroke patients quickly,” says Yanez, adding that UTMB provides care for more than 400 stroke patients a year. “Our record time for giving tPA is 18 minutes from the patient arriving in the ED to the needle puncture, and that’s amazing. Our goal is to always administer tPA in less than 60 minutes, and we continue to improve our numbers—our average is 40 minutes.”
I say goodbye to Yanez as she huddles with the ED staff to talk about next steps for the patient. After working in the ED for several years before becoming stroke coordinator, she feels right at home. The fast pace and time pressure are just par for the course.
“I love what I do—both the interaction with patients and caregivers,” she says. “We’re always working against the clock, but being part of a team that touches so many lives and provides positive outcomes keeps me energized.”