The Infant of the Diabetic Mother

Significant advances have been made in reducing perinatal mortality for the infant born to the mother with diabetes mellitus.
However, the infant of the diabetic mother (IDM) is likely to manifest a variety of problems, all of which require anticipation, recognition, and appropriate therapy.
Classification of Maternal Diabetes
Knowledge of the mother's diabetes, prior medical and pregnancy history, and complications during this pregnancy permits anticipation of many of the problems likely to be present in the postnatal period.
White's Classificaton permits assessment of severity of maternal diabetes. Classes B-H require medication.
Class A:
Chemical diabetes: positive glucose tolerance tests prior to or during pregnancy.
Prediabetes: history of large babies more than 4 kg or unexplained stillbirths after 28 weeks. Any age of onset or duration.
Class B: Onset after 20 years of age; duration less than 10 yrs.
Class C:
C1: Onset at 10-19 years of age.
C2: Duration 10-19 years.
Class D:
D1: Onset before 10 years of age.
D2: Duration 10 years.
D3: Calcification of vessels of the leg (macrovascular disease).
D4: Benign retinopathy (microvascular disease).
D5: Hypertension
Class E: Same as D, but with calcification of pelvic vessels.
Class F: Nephropathy
Class G: Many reproductive failures.
Class H: Diabetic cardiomyopathy
Class R: Malignant retinopathy
Class RF: Both nephropathy and retinopathy
Pedersen's prognostic signs of pregnancy permit more accurate predictions of poor outcome. These are: clinical pyelonephritis, precoma or severe acidosis, toxemia and neglectors (women who are uncooperative with the treatment plan.)
Maternal-Fetal Problems
Fertility
Diabetic women have normal fertility. In the first trimester there is an increased rate of spontaneous abortions. The incidence of these early losses varies with the diabetic classification:
Class A, 5-10% (not significantly different from the general population); Class B, 10%; Class C, 24%; Class D, 30%; and Class E, 74%.
Problems during pregnancy and delivery
- Episodes of hypoglycemia may occur in the first trimester, but it is not known whether these are associated with fetal damage.
- In the second trimester the insulin requirement increases, which is sometimes associated with ketoacidosis and resultant high fetal mortality.
- In the third trimester, the major problem is sudden, unexpected fetal death. Such deaths are sometimes associated with ketoacidosis, preeclampsia, or maternal vascular disease of the decidua and myometrium, but many are unexplained.
- Most diabetic pregnancies are associated with polyhydramnios. Although this is usually not a sign of significant fetal anomaly, it may be associated with premature rupture of membranes and early labor.
- In Classes A, B and C, the placenta and cord are usually large, but when vascular disease is present (as in Classes D E, and F) the placenta may be small and have multiple infarcts.
- The placenta has extramedullary hematopoiesis in diabetic pregnancies and this observation may be helpful in the postpartum investigation of the cause of late stillbirths.
Pregnancy Management
Good metabolic control of maternal diabetes improves the perinatal outcome.
Timing of delivery is individualized in each case and requires decision based on the risks of in utero fetal distress and stillbirth compared to the problems of prematurity.
Types of tests:
- Ultrasonography is a noninvasive method of estimating gestational age and assessing fetal growth.
- The lecithin-sphingomyelin ratio (L/S) or the shake test on amniotic fluid obtained by transabdominal amniocentesis can be utilized to predict pulmonary maturity.
- The oxytocin challenge test (OCT) and the non-stress test may predict impending fetal demise or the ability of the fetus to tolerate labor.
Evaluation of the Infant
Once the baby has been delivered, a careful assessment made on the basis of the Apgar score should indicate the need for any resuscitative efforts. In the delivery room, a screening physical examination for major congenital anomalies should be performed.
In the nursery, a more complete physical examination with special attention to the heart, kidneys, and extremities is performed. Close observation for potential problems should begin.
Specific Problems Encountered by the Infant
- Hypoglycemia
- Generally occurs in the first 24 hours and more often in infants of diabetic mothers taking insulin.
- Etiology is islet cell hyperplasia due to maternal hyperglycemia with subsequent hyperinsulinemia.
- Much less frequent with good maternal prenatal diabetic control.
- Respiratory Distress Syndrome. IDM's have about a six-fold increase risk of RDS when compared to infants of the same gestational age born to nondiabetic mothers. This is independent of the route of delivery (vaginal vs. c-section). The etiology is delayed pulmonary biochemical maturation.
- Hypocalcemia (< 7 mg/dl) occurs in 10-20% of IDMs, generally at 24-48 hours of age, and is more common (50%) if the mother takes insulin. This is due to transient hypoparathyroidism.
- Hypomagnesemia (< 1.5 mg/dl) may be seen in up to one-third of infants and correlates with severity of maternal disease.
- Polycythemia seen in 10-20%, may result from chronic hypoxia or as a result of too much stimulation of erythropoietin production by hyperinsulinemia
. - Hyperbilirubinemia (non-physiologic) is seen in about 20%, and is due to polycythemia, decreased red cell survival and delayed clearance of bilirubin load.
- Congenital malformations are more likely to occur in IDMs than in normal babies, and the incidence increases with increasing duration and severity of maternal diabetes. Malformations account for about half of the perinatal mortality seen in the IDM, and include congenital heart disease, renal anomalies, vertebral dysplasia, cleft lip/palate, orthopedic anomalies, and caudal regression syndrome.
- Renal vein thrombosis presents with hematuria and a flank mass. The etiology is unknown.
- Small left colon syndrome presents with abdominal distension. Contrast enema shows a small left colon. Meconium passage following the enema usually resolves the symptoms.
- Diabetic cardiomyopathy presents with respiratory distress and symptoms of congestive failure. These babies have asymmetric septal hypertrophy with secondary left ventricular outflow tract obstruction resembling idiopathic hypertrophic subaortic stenosis. It correlates with poor maternal control resulting in fetal hyperinsulinemia. Digoxin is contraindicated; the drug of choice for symptomatic babies in congestive failure is propranolol.
- Macrosomia and birth injury due to difficult delivery. The risk for brachial plexus injury, facial palsy, intracranial hemorrhage (subdural), clavicular fractures, phrenic nerve paralysis, hemorrhage into abdominal organs (especially liver and adrenals) is increased.
- Asphyxia due to reduced uteroplacental blood flow or placental edema may occur.
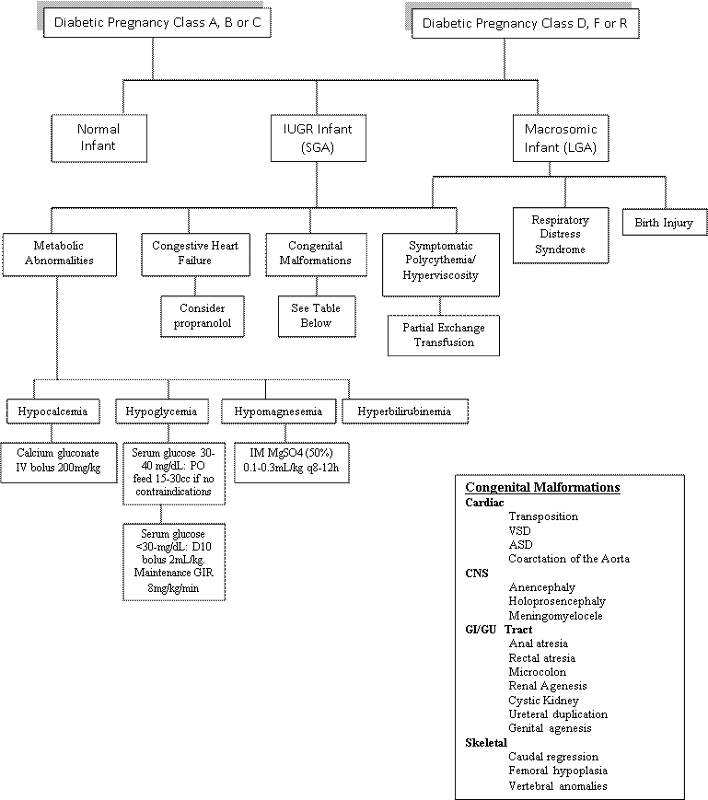
Critical Paths for the Infant of a Diabetic Mother
toc | return to top | next page

