Sprains
A sprain is an injury to a ligament which is a band of short, fibrous connective tissue that connects between two bones or bone to cartilage to stabilize a joint together with other ligaments.
|
Sprain Severity Grading System Note that the time for healing of a sprain is not always proportional to the grade of the spran. |
|---|
|
Grade I sprain a. Mild stretching of a ligament with no or microscopic tears b. Mild tissue swelling and tenderness c. No joint instability or laxity on examination d. Able to bear weight and ambulate with minimal pain |
|
Grade II sprain a. An incomplete tear of a ligament b. Moderate pain, with soft tissue swelling, an effusion tenderness, and ecchymosis c. Mild to moderate joint instability with some restriction of the range of motion and loss of function d. Painful weight bearing and ambulation e. Require external support such as a brace or splint |
|
Grade III sprain a. A complete tear of a ligament b. Severe pain, swelling, tenderness, and ecchymosis c. Significant mechanical instability and loss of function and motion on examination d. Unable to bear weight or ambulate e. May require prolong external support for healing or sometimes surgery |
Ankle Sprains
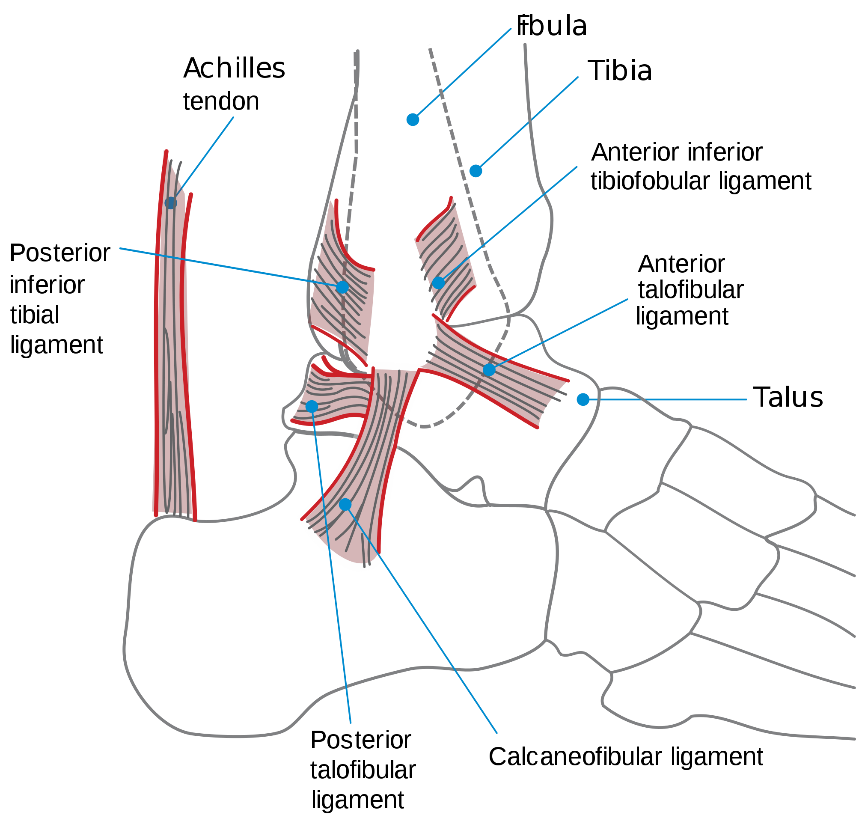
Image source from Wikimedia Commons: https://commons.wikimedia.org/wiki/File:Ankle_en.svg
Lateral ankle sprain
Mechanism of Injury
- Caused from inversion of the plantar-flexed foot
- Anterior talofibular ligament (ATFL) - most common; it is located anterior to the lateral malleolus and proximal to the ankle joint
- Calcaneofibular ligament (CFL)
- Posterior talofibular ligament
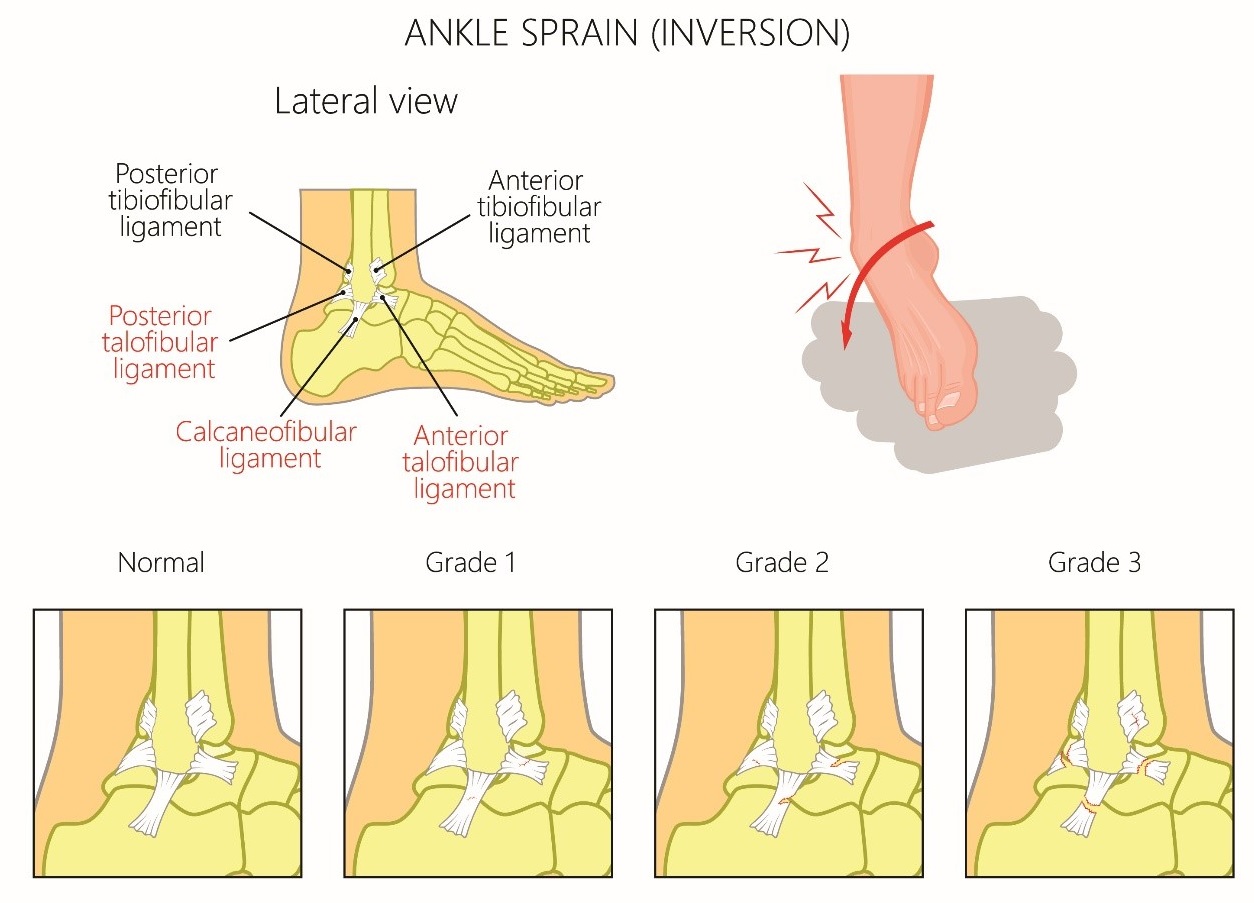
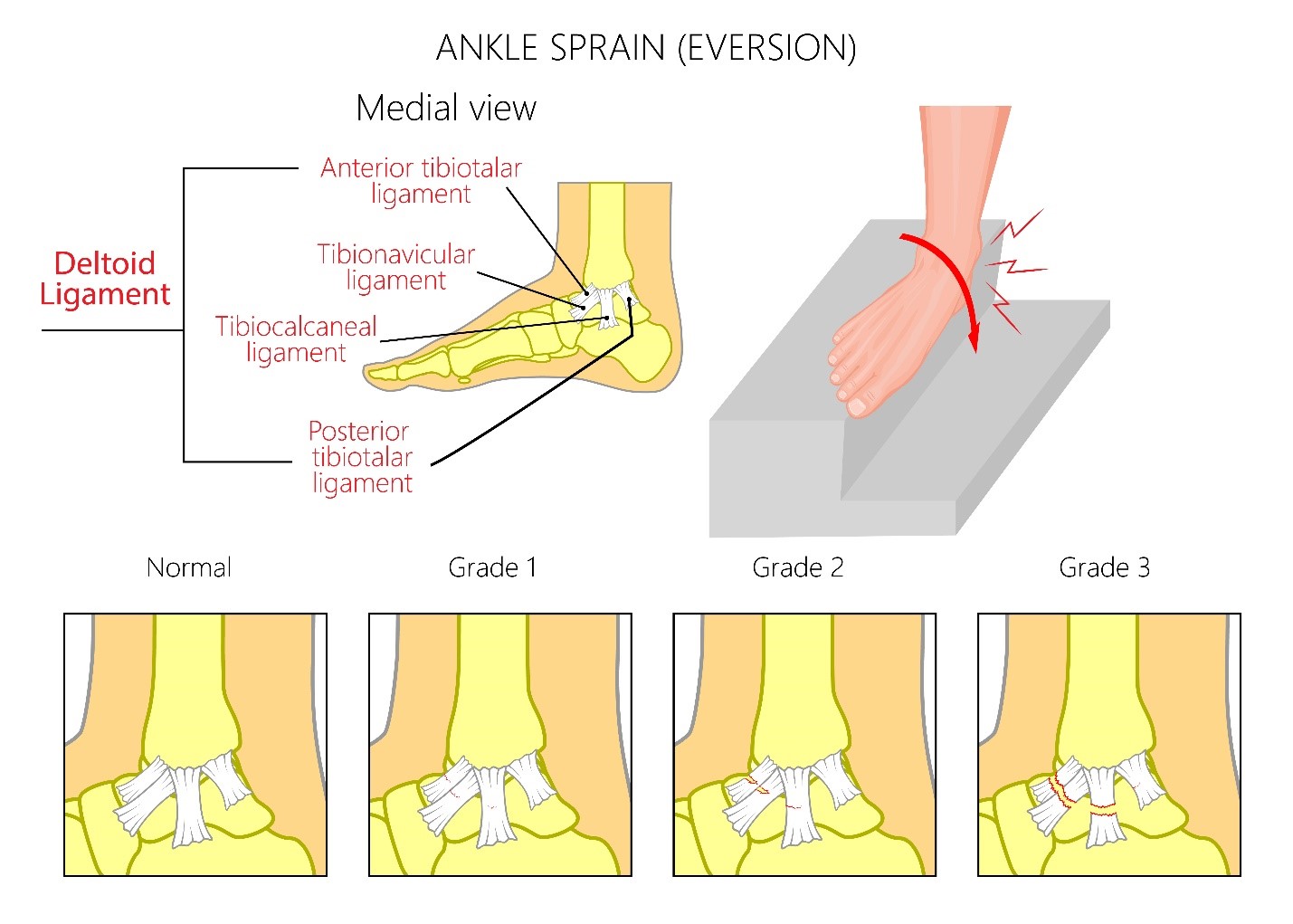
Medial ankle sprain
- Caused by forced eversion to the deltoid ligament, consisting of anterior tibiotalar ligament, posterior tibiotalar ligament, tibionavicular ligament, and tibiocalcaneal ligament
- Due to the strong nature of the deltoid ligament, it is more common to see an avulsion fracture of the medial malleolus.
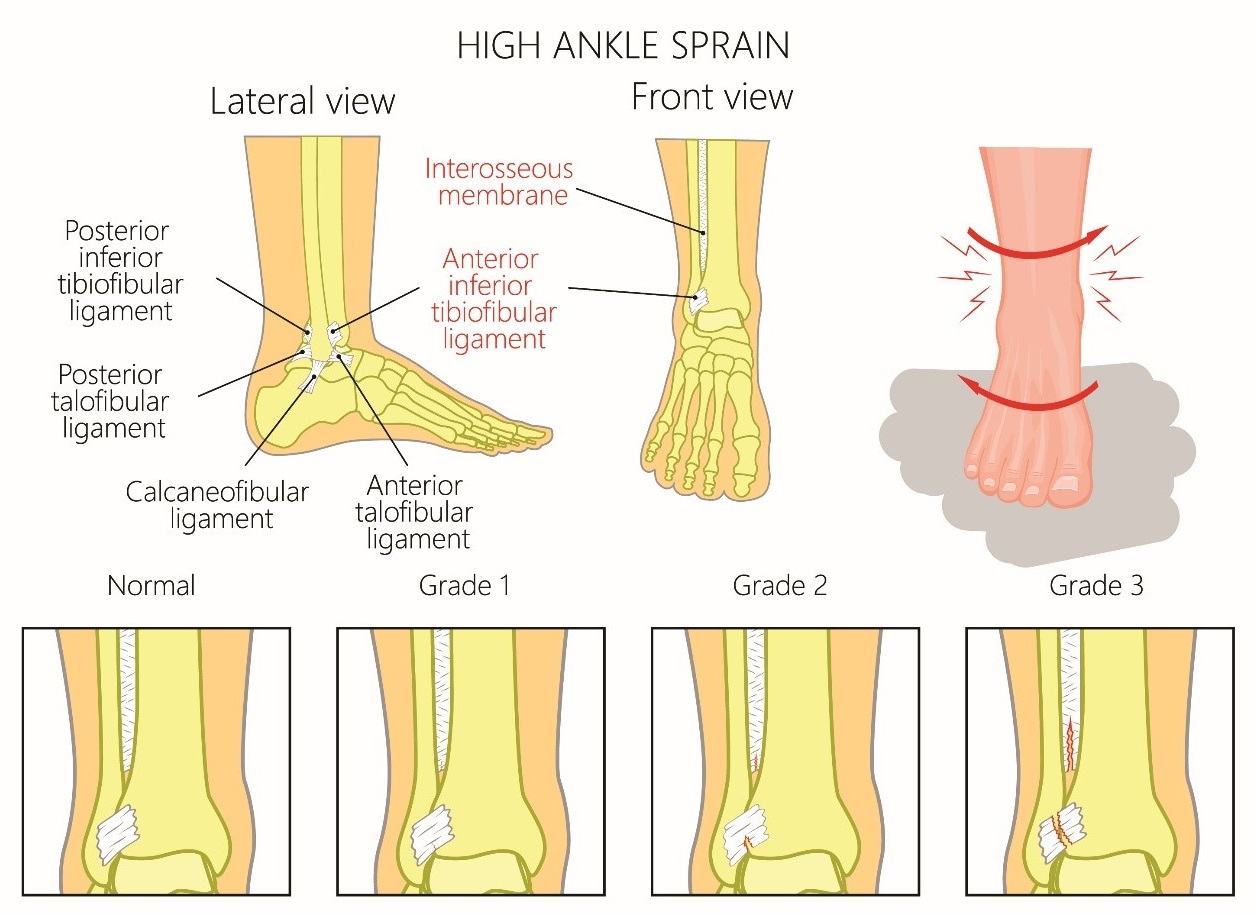
Syndesmotic (high-ankle) sprain
- Occurs with forced dorsiflexion and eversion (e.g. a child jumps from a height, slides into a base, or decelerates while skiing).
- The syndesmosis is the membrane between the distal tibia and fibula.
Physical Examination
Physical exam should start with an inspection for swelling, ecchymosis and tenderness in the areas required for the Ottawa ankle rules (discussed below), and laxity of ankle ligaments, assessment for effusion, evaluation of range of motion including ambulation and neurovascular status, and comparison of the injured with the uninjured side.
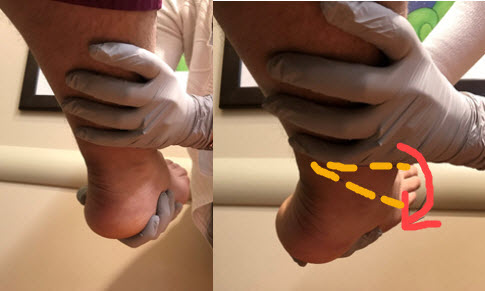
Anterior Drawer Test
The test assesses the integrity of the ATFL. An examiner holds the lower leg with one hand and, while gripping the heel with the other hand, pulls anteriorly. Anterior displacement of the heel beneath the ankle in comparison with the contralateral side indicates a tear of the ATFL.
Talar Tilt Test
Inversion of the heel assesses the stability of the CFL. Eversion of the heel to assesses the integrity of the deltoid ligament.
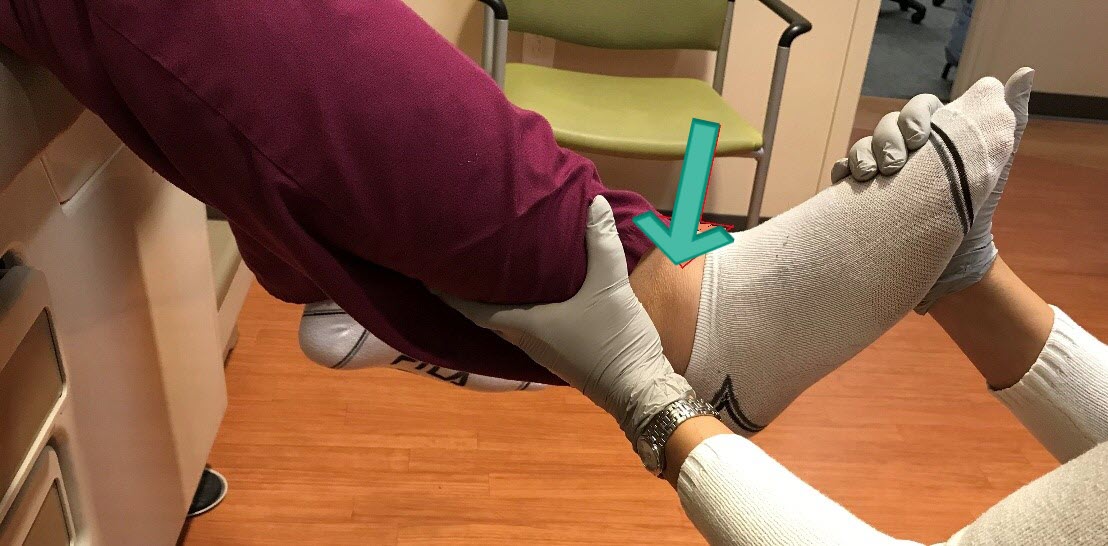
Tibia-Fibula Squeeze Test
The test identifies a syndesmotic sprain. It is a positive test when there is pain anterior and proximal to the ankle joint upon squeezing the tibia against the fibula at mid-calf. An orthopedist should be consulted for a syndesmotic sprain because surgery may be needed to maintain joint integrity and stability.
External Rotation Stress Test
This test also identifies a syndesmotic sprain. It is a positive test if pain is elicited in the region of the ATFL when the clinician stabilizes the leg proximal to the ankle joint, while grasping the plantar aspect of the foot and rotating the foot externally relative to the tibia.
Evaluation: Imaging
|
Ottawa Ankle Rules were created to limit unnecessary radiographs and are sensitive in children older than six years of age. An ankle series is recommended only if: Pain in the malleolar zone AND bony tenderness at the posterior edge or tip of the lateral or medial malleolus OR |
X-rays: in children, ligaments are stronger relative to their bones, and may need to rule out an underlying fracture first by radiography which should include antero-posterior, lateral, and oblique views.
A foot series is recommended only if there is pain in mid-foot zone AND any of the following findings:
- bony tenderness at the base of the fifth metatarsal
- bony tenderness at the navicular bone
- inability to bear weight both immediately and in the emergency department.
Computed tomography may be used to rule out occult fracture.
MRI may be required for ankle pain not resolved after 6-8 weeks.
Management
a. Immobilization
Grade I sprain: An elastic (ace) wrap for a few days
Grade II sprain: The combination of an elastic wrap and an aircast for up to a few weeks
Grade III sprain: Ankle splints or below the knee cast for a brief period of immobilization followed by functional rehabilitation with gradual increase intensity by physical therapy
Referral to the orthopedist is beneficial, since surgery is sometimes considered in some patients with repeated large stresses on ankle joints.
b. Supportive Care: Immediate therapy - "RICE" treatment for the first two to three days
Rest: avoid movements/activities that can reproduce pain, use crutches.
Ice: apply on the affected area every 2-3 hours for 15-20 minutes each time for the first 48 hours or until swelling is improved. Place thin towel between the ice and skin.
Compression: wrap the affected joint with an elastic bandage to help support the joint and minimize swelling.
Elevation: raise the affected joint above the level of the heart.
c. Pain Control - Nonsteroidal anti-inflammatory drugs (NSAIDs) or non-NSAID analgesics
Wrist Sprains
Wrist sprains involve injury to the supporting ligaments of the radiocarpal joint. Wrist sprains are rare in children but may occur in adolescent athletes who experience twisting injuries.
Mechanism of Injury
Scapholunate ligament sprains - result from excessive wrist extension with pronation (eg, a fall on an extended wrist). This is the most common of the wrist sprains.
Lunotriquetral sprains - result from sudden axial loading with wrist extension and radial deviation, causing pain along the ulnar aspect of the wrist.
Ulnar collateral ligament sprains - occur during forced hyperextension and abduction, also known as gamekeeper's thumb or skier's thumb.
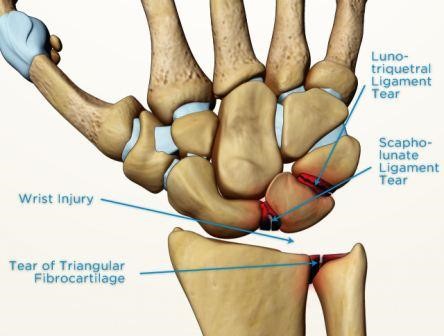
Image Source: https://www.sportsmd.com/sports-injuries/wrist-hand-injuries/scapholunate-ligament-tear/
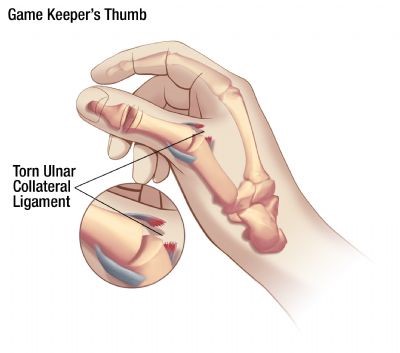
Image Source: https://www.aliem.com/2013/07/ulnar-collateral-ligament-injury/
Physical Examination
Physical exam should start with an inspection in the areas for tenderness, swelling and ecchymosis, assessment for effusion, evaluation of range of motion and neurovascular status, and comparison of the injured with the uninjured side.
- For scapholunate ligament injury: swelling, audible clicks, tenderness out of proportion to injury, decreased range of motion, decreased grip strength
- For lunotriquetral ligment injury: ulnar wrist tenderness, weakness, and a clicking sound
- For ulnar collateral ligament injury: pain is felt on the ulnar side of the metacarpophalangeal joint of the thumb, especially with valgus stress
Evaluation: Imaging
X-ray findings may be normal or show an increased scapholunate distance. X-ray findings are usually normal in lunotriquetral sprains.
Management
The primary goals of sprain management are to reduce swelling and inflammation.
a. Immobilization
- Scapholunate injury: thumb spica splint
- Lunotriquetral injury: ulnar gutter splint
- Ulnar collateral ligament injury: thumb spica splint and complete rest for three weeks, followed by passive range of motion exercises with continued splinting for several more weeks.
b. Supportive Care
- Mild to moderate sprains - "RICE" treatment for the first few days.
- Pain control - Nonsteroidal anti-inflammatory drugs can be prescribed for inflammation and pain.
c. Referral to a hand specialist should be considered because untreated ligamentous injuries to the wrist may result in chronic pain and functional compromise. Orthopedic referral is recommended for scapholunate ligament injury.
QuickCheck

