Arrhythmias
Arrhythmias are defined as disturbances in heart rate and/or conduction. Arrhythmias result from abnormal impulse formation, abnormal impulse conduction, or both. Arrhythmias may occur in children with normal hearts and/or may be associated with CHD, medications or electrolyte disturbances.
Bradyarrhythmias
Sinus bradycardia
The normal range of heart rate depends on the age of the individual, ranging from 120-160 beat/min in the newborn to 60-80 beat/min in the adult. Trained athletes may normally have sinus bradycardia due to increased vagal tone. Pathological sinus bradycardia is usually secondary to an underlying condition such as hypothyroidism or medications such as beta-blockers.
Asymptomatic physiologic sinus bradycardia requires no treatment. In symptomatic bradycardia, the underlying cause should be treated and a pacemaker placement may be considered if there is no response to medical therapy.
Atrioventricular Block
First degree AV block
This indicates prolongation of the PR interval more than 95th percentile for age and heart rate and is due to impairment in the AV node conduction caused by increased vagal tone, AV nodal ischemia or drugs such as digoxin and beta-blockers. It is usually reversible and does not require any treatment. First degree A-V block could be one of the cardiac manifestations of rheumatic fever (Figure).
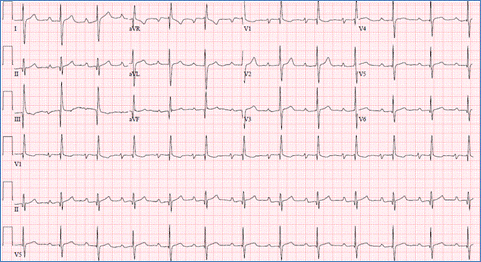
Figure demonstrating an EKG with first degree AV block
Second degree AV block
This is secondary to an intermittent failure of conduction through the AV node so that some P waves are not followed by QRS complexes.
Mobitz type I (Wenckebach) is gradual prolongation of the PR interval until there is a complete block (a P wave not followed by a QRS complex). This is due to impaired conduction through the AV node and is usually benign. This may be seen in the presence of increased vagal tone, in trained athletes and during sleep (Figure).
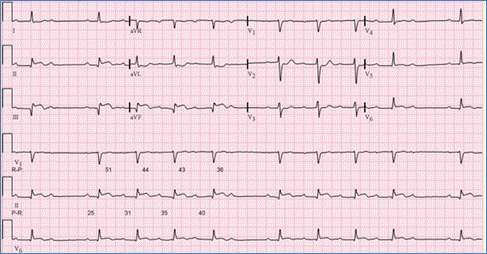
Figure demonstrating an EKG with Mobitz type I second degree AV block
Mobitz type II is sudden loss of AV conduction (two or more P waves before QRS complexes). It is more serious as it may progress to a complete AV block. Implantation of a pacemaker may be considered in symptomatic patients.
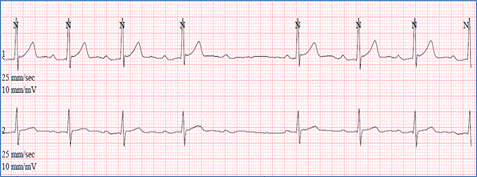
Figure demonstrating an EKG with Mobitz type II second degree AV block
Third degree AV block
Complete AV block represents complete atrioventricular dissociation with no correlation between the atrial and ventricular electrical activity. The ventricular rate is significantly slower than the atrial rate. A pacemaker placement is warranted in symptomatic patients (Figure).
This condition may be seen in infants born to mothers with systemic lupus erythematosus (SLE).
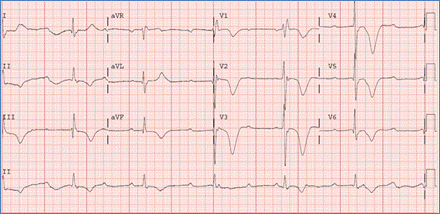
Figure demonstrating an EKG with third degree AV block
Tachyarrhythmias
Sinus tachycardia
Sinus tachycardia is characterized by narrow fast QRS complexes that are preceded by normal P waves (Figure). The heart rate depends on patient age and may reach up to 220 beat/min in neonates. Sinus tachycardia may be a physiologic response to exercise, anxiety, fever, hypovolemia, hypoxemia or hyperthyroidism.
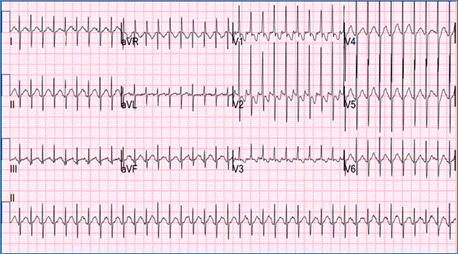
Figure demonstrating an EKG with sinus tachycardia (presence of P waves)
Premature atrial complexes (PACs)
PACs represent origination of atrial electrical activity outside the SA node. On the EKG, PACs may appear in one of three forms:
- Premature P wave followed by a narrow QRS complex (conducted PAC) (Figure).
- Premature P wave not followed by a QRS complex (nonconducted PAC).
- Premature P wave followed by wide QRS complex (conducted PAC with aberrancy i.e. bundle branch block).
PACs are commonly seen in infants and disappear with increasing age. This arrhythmia is usually benign and needs no treatment.
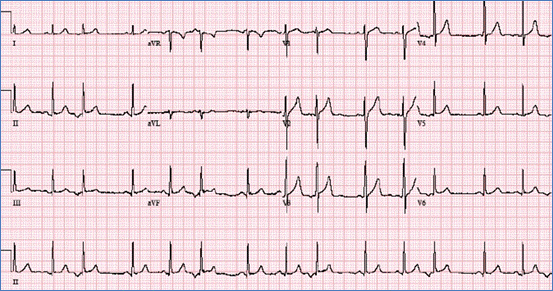
Figure demonstrating an EKG with PAC
Atrial Flutter and Atrial Fibrillation
Atrial flutter is characterized by rapid atrial activity at a rate of 200- 350 beat/min. The P waves have saw-tooth appearance. Some of the atrial impulses are not conducted through the AV node, so the ventricular rate is slower than the atrial rate and is usually regular. Atrial flutter is caused by a reentry circuit in the atrium and is usually seen in a diseased heart. The symptoms depend on the ventricular rate. Cardioversion is indicated in symptomatic patients.
Atrial fibrillation is a chaotic atrial rhythm (300-600 impulses per minute) with no well-defined P waves. The ventricular rate is irregularly irregular. Atrial fibrillation usually requires treatment with antiarrhythmic medications such as beta-blockers or Ca++ channel antagonists. Systemic anticoagulation is usually needed to reduce the risk of thrombus formation in the fibrillating atrium and downstream embolization.
Supraventricular Tachycardia (SVT)
SVT is characterized by a narrow QRS complex tachycardia with a heart rate of 250-350 beat/min that shows no variation with respiration (Figure). It is commonly seen in normal children but may be associated with some CHD such as Ebstein anomaly. SVT is usually caused by an accessory pathway between the atria and the ventricles, or by a reentry circuit within the AV node.
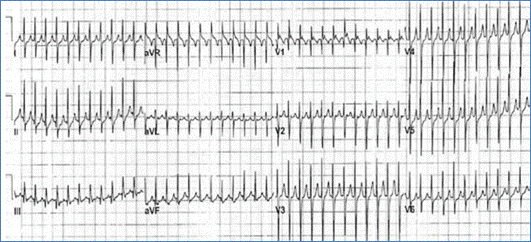
Figure demonstrating an EKG with SVT (no P waves are seen)
In infants, SVT presents with poor feeding, irritability, sweating and respiratory distress. If not treated, CHF and death may occur.
Compensated SVT should be treated promptly with vagal maneuvers such as application of ice to the face. If this is unsuccessful, then adenosine should be administered intravenously. Children with uncompensated SVT should undergo cardioversion.
WPW syndrome is an example of pre-excitation due to an accessory pathway between the atria and ventricles (Figure). It is characterized by short PR intervals, delta waves, and wide QRS complexes.
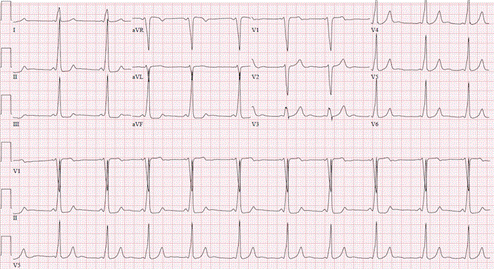
Figure demonstrating an EKG with Wolff Parkinson White syndrome
Ventricular arrhythmias
Ventricular arrhythmias are characterized by wide QRS complexes and abnormal T waves. The symptoms depend on the heart rate and are usually due to poor ventricular filling. This is a serious dysrhythmia and synchronized cardioversion is commonly indicated.
Premature ventricular contractions (PVCs)
PVCs are premature, wide QRS complexes that are not preceded by P waves (Figure). Isolated unifocal PVCs originate from the same spot in the ventricles as they have uniform morphology. They are usually benign in nature and disappear with exercise. Multifocal PVCs have different morphology as they originate from different foci in the ventricles. They usually occur in diseased myocardium and often increase with exercise. If they increase with exercise, further electrophysiologic testing is usually required.
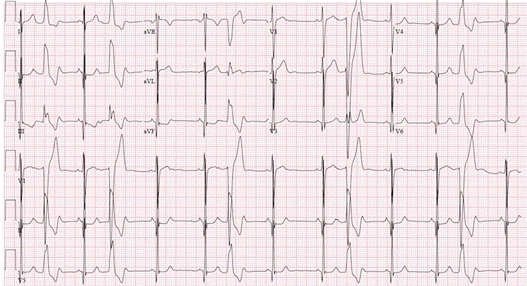
Figure demonstrating an EKG with Premature Ventricular Complexes
Ventricular tachycardia (VT)
VT is a rapid, wide QRS-complex tachycardia with a heart rate 150-250 beat/min (Figure). It is a serious condition that may result from drug toxicity (digoxin), myocarditis or severe metabolic derangement. It should be treated promptly with cardioversion if the patient is hemodynamically unstable. Stable VT may be treated with IV lidocaine infusion. Oral amiodarone may be used for outpatient management.
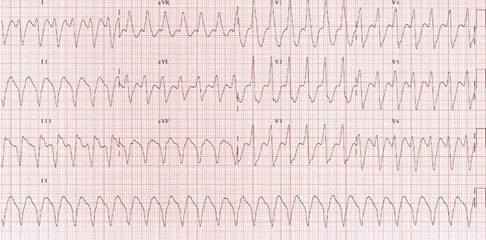
Figure demonstrating an EKG with Ventricular Tachycardia
Ventricular Fibrillation (VF)
VF is a terminal cardiac rhythm characterized by irregular wide bizarre shaped QRS complexes (Figure). It needs to be treated immediately with unsynchronized DC cardioversion.
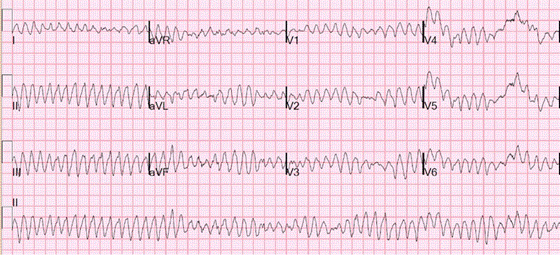
Figure demonstrating an EKG with Ventricular Fibrillation


