Kawasaki Disease (Mucocutaneous Lymph Node Syndrome)
Kawasaki Disease (KD) is an acute multi-system immune-mediated vasculitis of unknown etiology. It usually presents in infancy and early childhood with 85% of those affected are less than 5 years of age. KD is the leading cause of acquired heart disease in children in the US. In untreated KD patients, the incidence of coronary artery aneurysm ranges from 15-25%. Myocardial infarction from thrombotic occlusion of the coronary arteries is the principle cause of death. KD is more common in patients of Asian descent. The prognosis depends on the extent of the cardiac involvement and the promptness of medical treatment.
Pathogenesis
The etiology of KD is unknown. The inflammation in KD involves small to medium-sized arteries, including the coronary arteries. The extent of the coronary artery involvement is the critical factor that determines morbidity and mortality. Investigators propose that mediators such as tumor necrosis factor (TNF), interleukin (IL)-1B, interferon (INF) and IL-6 produced by activated T-cells and macrophages promote vascular injury. The earliest pathological change reported in the vessel wall is subendothelial accumulation of T-cells, mononuclear cells, macrophages and monocytes.
Clinical presentation
KD is divided into three phases.
- The acute phase begins with the onset of a high fever without an apparent source that may last for 1-2 weeks. Acute myocardial infarction may occur during the acute phase due to vasculitis and perivasculitis.
- In the subacute phase, which may last for 2-4 weeks, the fever subsides. Desquamation of the skin and coronary artery aneurysms may appear in this phase. The platelet count increases and may rise above 106 per mm3. Other acute phase reactants such as ESR and CRP are usually elevated.
- During the convalescent phase, the symptoms resolve and the platelet count and ESR return to normal, usually within 6-8 weeks following onset of the illness.
Making the Diagnosis
According to U.S. and Japanese guidelines, Kawasaki disease is a clinical diagnosis.
Classic KD is diagnosed by the following criteria:
- Fever of unknown origin lasting for at least 5 days, in addition to four of the following criteria:
- Bilateral conjunctivitis which is non-purulent
- Changes of the oral cavity and lips: cracked and erythematous lips, strawberry tongue
- Changes in the extremities (erythema of the hands and feet, desquamation of the skin of the fingers and toes in the 2nd and 3rd weeks)
- Polymorphous rash: maculopapular, erythema multiforme-like or scarlatiniform rash, involving extremities, trunk, and perineal regions
- Cervical lymphadenopathy (> 1.5 cm in diameter) that is commonly unilateral
- Alternative diagnostic criteria : Fever for at least five days and two or three of the clinical features or coronary artery abnormalities on transthoracic echocardiography
- Supplementary laboratory criteria (not required for diagnosis):
- Anemia
- Cerebrospinal fluid pleocytosis
- Elevated C-reactive protein and erythrocyte sedimentation rate
- Elevated liver enzyme levels
- Hypoalbuminemia < 3.0 g/dl
- Hyponatremia
- Platelets > 450 per mm3 after first week
- Sterile pyuria
- White blood cell count > 15,000/uL
- Incomplete (Atypical Kawasaki Disease)
In some cases, patients do not fulfill the classic criteria for Kawasaki disease and are classified as having incomplete (atypical) disease. Incomplete disease is more common in younger infants and older children and should be suspected when patients have a fever for at least five days with only two or three of the principal clinical features. As a result, it is important to consider the diagnosis of Kawasaki disease and the possible need for echocardiography in all children who have an unexplained fever lasting at least seven days with laboratory evidence of systemic inflammation .
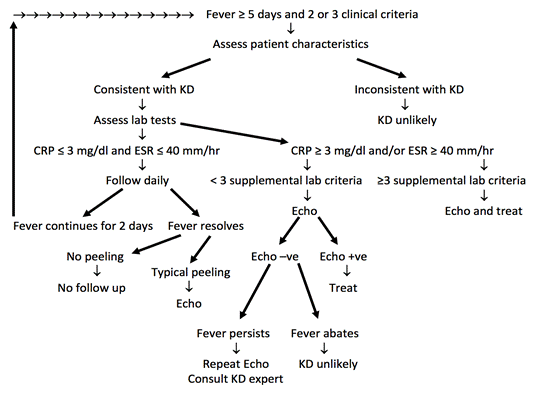
Figure demonstrating a suggested algorithm for the management of suspected Kawasaki Disease
Other clinical signs:
- Tachycardia and gallop rhythm (secondary to myocarditis) may occur.
- Pericardial effusion, aortic regurgitation, and mitral regurgitation may be seen.
- EKG shows mild abnormalities consistent with myocarditis such as arrhythmias, prolonged PR and QT intervals and nonspecific ST segment changes.
- Echo may show pericardial effusion, LV dilation, mitral insufficiency and/or decreased systolic function. Follow up echo should be done in 3-5 weeks. The need for further echocardiograms is determined by the presence or absence of coronary involvement.
- Coronary angiography should not be done in the acute phase but may be needed later on to evaluate the extent of the coronary involvement.
- Stress test may be needed in teenagers who had a history of previous coronary involvement before participating in competitive sports
Management (Figure):
Early detection of KD and prompt treatment reduce mortality below 1%. Baseline echocardiogram should be performed as soon as the diagnosis is made. The table below helps to stratify the risk of patients with KD and helps determine follow up testing.
1.Treatment of Acute Disease:
- A single IVIG (2 g/kg).
- High dose aspirin 80-100 mg/kg/day in 4 doses for at least 48-72 hours after cessation of fever; low dose should continue at 3-5 mg/kg/ day for 6-8 weeks until the acute phase reactants normalize and a repeat echo is negative for coronary involvement.
- Corticosteroids – not well established though some studies have shown shorter duration of symptoms and decreased severity of coronary involvement
- Pentoxifylline "an inhibitor of TNF-alpha RNA transcription" has been shown to be effective as adjunctive therapy but its true role in treatment is yet to be determined.
- Children should be vaccinated against varicella and influenza and the physician should be contacted immediately if the child has been exposed to the wild type of the virus.
- Measles and varicella vaccines should be avoided for 11 months following administration of high dose IVIG.
2. Treatment of Refractory Disease:
- Failure of IVIG therapy occurs in up to 10% of patients with KD and is defined as persistence of fever more than 36 hours after treatment with IVIG.
- Even with high dose IVIG ~ 5% of patient may develop coronary dilation (ectasia) and ~ 1% may develop coronary aneurysms.
- Retreatment
- A second dose of IVIG is recommended (2 g/kg).
- Pulse methylprednisolone 30 mg/kg for 2-3 hours administered once daily for 1-3 days (one study states that treatment should be monitored with CRP levels).
- Abciximab may be considered in cases where large aneurysms are present in the acute and subacute phase.
- Patients with moderate sized aneurysms are treated with aspirin in combination with other antiplatelet agents such as clopidogrel (Plavix) or dipyridamole (Persantine).
- A combination of aspirin and LMWH or warfarin may be used in thrombosis prophylaxis and treatment.
- Cardiac catheterization is recommended for patients with angina pains or ischemic changes on a stress test. It may be used as a diagnostic and interventional tool.
- Surgical intervention may be considered for significant ischemia/stenosis that is not amenable to catheterization.
3. Follow up of KD
- Aneurysms need to be followed with serial echocardiograms until they completely subside.
- Exercise stress test may be considered in select patients.
- Patients with regression of the coronary aneurysms remain at risk for stenosis because the affected area may be less compliant.
- Patients with coronary involvement without aneurysm development may still be at higher risk for altered lipid metabolism and early development of atherosclerosis.
- Risk stratification (see Table below)
|
Risk Level |
Pharmacological Therapy |
Physical Activity |
Follow-up and Diagnostic Testing |
Invasive Testing |
|---|---|---|---|---|
|
I (No coronary artery changes at any stage of illness) |
None beyond 1st 6-8 weeks |
No restrictions beyond 1st 6-8 weeks |
Cardiovascular risk assessment, counseling at 5-y intervals |
None recommended |
|
II (transient coronary artery ectasia, disappears within 1st 6-8 weeks) |
None beyond 1st 6-8 weeks |
No restrictions beyond 1st 6-8 weeks |
Cardiovascular risk assessment, counseling at 3- to 5-y intervals |
None recommended |
|
III (1 small-medium coronary artery aneurysm / major coronary artery) |
Low-dose aspirin (3-5 mg/kg aspirin per day), at least until aneurysm regression is documented |
For patients <11 y old, no restriction beyond 1st 6-8 weeks: patients 11-20 y old, physical activity guided by biennial stress test, evaluation of myocardial perfusion scan; contact or high-impact sports discouraged for patients taking antiplatelet agents
|
Annual cardiology follow up with echocardiogram + EKG, combined with cardiovascular risk assessment, counseling; biennial stress test/evaluation of myocardial perfusion scan |
Angiography, if noninvasive test suggests ischemia |
|
IV (≥ 1 large or giant coronary artery aneurysm, or multiple or complex aneurysms in same coronary artery, without obstruction |
Long-term antiplatelet therapy and warfarin (target INR 2.0-2.5) or low-molecular-weight heparin (target: anti-factor Xa level 0.5-1.0 U /mL) should be combined in giant aneurysms |
Contact or high-impact sports should be avoided because of risk of bleeding; other physical activity recommendations guided by stress test/evaluation of myocardial perfusion scan outcome |
Biannual follow-up with echocardiogram + ECG; annual stress test/evaluation of myocardial perfusion scan |
1st angiography at 6-12 mo or sooner if clinically indicated; repeated angiography if noninvasive test, clinical or laboratory findings suggest ischemia; elective repeat angiography under some circumstances (see text)
|
|
V (coronary artery obstruction) |
Long-term low-dose aspirin; warfarin or low-molecular-weight heparin if giant aneurysm persists; consider use of β-blockers to reduce myocardial o2 consumption |
Contact or high-impact sports should be avoided because of risk of bleeding; other physical activity recommendations guided by stress test/myocardial perfusion scan outcome |
Biannual follow-up with echocardiogram and ECG; annual stress test/evaluation of myocardial perfusion scan |
Angiography recommended to address therapeutic options |
References
American Academy of Pediatrics.
Diagnosis, Treatment, and Long-Term Management of Kawasaki Disease: A Statement for Health Professionals from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, American Heart Association. Pediatrics 114 (6) December 2004, pp. 1708-1733 (doi:10.1542/peds.2004-2182)
Sanchez-Manubens J, Bou R, Anton J. Diagnosis and classification of Kawasaki Disease. Journal of Autoimmunity. 48-49 (2014) 113-117


