Additional Questions You May Have About Healthcare Quality
Click on the question to expand/collapse the answer:
+/- What are UTMB's guiding principles for quality reporting?
Our Guiding Principles
Achieving Highly Reliable Care
These are the guiding principles we follow to achieve and invest in high-reliability health care:
- We define quality as achieving optimal health outcomes and patient experiences at an affordable cost. We do this by focusing on safe, timely, effective, efficient, equitable, patient-centered, and evidence-based care. We continually work to improve in these areas.
- No matter how well we perform or how much we improve, we will always work harder to enhance the quality of the care we deliver. We will always apply new knowledge and better ways to enhance outcome and remain vigilant to assure patients’ safety. We aspire to make each patients’ experience of care positive and healing.
- We will use the appropriate resources for diagnosis and treatment and not more than is needed.
- We will enhance our patients’ and their families’ experience of care by effectively communicating and through shared decision-making.
- Innovations and improvements are proactive, data-driven and continuously monitored.
Quality Measurement and Reporting
Generally, a few principles guide UTMB’s approach to measurement and reporting:
- Publication of performance results or pay-for-performance initiatives should only employ measures that have been vetted after thorough third party testing and validation (e.g. the National Quality Forum, a broad-based national clearinghouse). Anything less seems irresponsible.
- Health care decisions are better informed when patients and their doctors discuss the match of their specific needs with the skills and services of their provider using tools like
- The calculations used to measure our data must be conceptually coherent and statistically sound.
- We must be transparent with our data by also communicating any issues involved in measuring our performance.
+/- Where does the data come from?
Where does the datas come from?
Most publicly reported data is obtained through billing information. Billing information is a summary of the care that was received during the hospital stay or clinic visit. This information does not provide the details of the care provided, which is more useful when trying to improve the health care patients receive.
By participating in national programs, UTMB is able to benchmark itself against other organizations to identify areas for improvement. These national programs allows for organizations to share best practices so that improvements made at one facility can be duplicated with all those participating. This ensures that patients receive the best possible care at the lowest cost.
+/- How does UTMB calculate its star ratings?
Understanding the 5-Star Rating Scale
Data about health care quality data can sometimes be complex and difficult to understand. To help make it easier for viewers to understand how well we our performing compared to our peers, we have used a 5-star rating system. A greater number of stars means that our outcomes are better. However, three stars means that our outcomes are average compared to other similar hospitals.
How we calculate ratings:
When comparing our quality metrics to our peers, we calculate our ranking by using the following the following method:
- Determine the total number of hospital included in the group.
- Place all of the hospitals in the group in order from best to worst performers.
- Determine where we rank among our peers by percentile.
For example, if there were 100 hospitals in the group, and UTMB ranked in 24th place, UTMB’s percentile ranking would be calculated as follows:
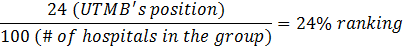
Once our percentile ranking is determined, we use the following star rating system to determine our star rating:
★ ★ ★ ★ |
|
| ★ ★ ★ ★ | Compared to other hospitals, UTMB is in the top 1-20% of performers for this measure. Stated differently, if there were a race with 10 racers, UTMB would be placed 1st or 2nd. |
| ★ ★ ★ | Compared to other hospitals, UTMB is in the 41-60% of performers. Stated differently, if there were a race with 10 racers, UTMB would be placed 5th or 6th. |
| ★ ★ | Compared to other hospitals, UTMB is in the 61-80% of performers for this measure. Stated differently, if there were a race with 10 racers, UTMB would be placed 7th or 8th in the race. |
| ★ | Compared to other hospitals, we’re in the 81-100% of performers for this measure. Stated differently, if there were a race with 10 racers, UTMB would be placed 9th or 10th in the race. |
How we calculate provider ratings:
The physician rating is calculated slightly differently and is given for the providers in the clinics (doctor’s office) only. It provides a quick reference to see how patients rated the care of that provider during the last 12 months. A group of patients (randomly selected) are sent a survey by Press Ganey (link to Press Ganey) that asks seven questions about the care they got from their provider.
One question asks patients to rate their provider overall from 0-10. To obtain a star rating for each provider, the answers are first added together and then divided by the total number of answers to get an average score. Since the answers range from 0-10, but our stars only range from 0-5, we then divide that average score by two to get the star rating. For example, if seven surveys were returned and the scores were 10, 9, 9, 9, 9, 9, and 8, the score would be calculated using the following steps:
- Add the survey scores together for the question to get an average score.
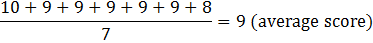
- Divide the average score by 2 (to change the number to a score of 0-5).
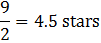
|
Patient Answer |
Physician Score |
No |
0.0 |
Yes, somewhat |
2.5 |
Yes, definitely |
5.0 |
+/- What does UTMB publicly report ?
What does UTMB Publicly Report?
Click here to see our reports.
Data for this information can also be found on Hospital Compare, but please because there is a delay between the time that the data is submitted to the Centers for Medicare and Medicaid (CMS) and the time it is published on their website, we post our most recent performance data on this website. Information is updated on a quarterly annual basis.
+/- Where can health care consumers view these reports?
Where can health care consumers view these reports?
As a health care consumer, there are places you can go to find information about the quality of care we deliver at UTMB. One important way to learn about hospital quality is to look at hospital report cards developed by state and consumer groups, like Hospital Compare. A recent study about such reports found that in addition to helping consumers make informed choices, they also encourage hospitals to improve their quality of care.
Hospital Compare: The U.S. Department of Health & Human Services is a website designed for the public to compare hospitals in their surrounding area. Visit the Hospital Compare for more information.
+/- How are academic medical centers different from other hospitals?
How are academic medical centers different from other hospitals?
As a regional hospital service provider, we offer a wide range of services and may receive patients who need special care that other hospitals can’t provide. As an academic medical center (AMC), we also are home to four schools: a school of medicine, school of nursing, school of health professions, and a graduate school of biomedical sciences.
As a part of our mission, UTMB:
- educates future doctors and other health professionals,
- conducts medical research, advancing innovations in care, and
- provides service to the community, especially underserved populations.
UTMB provides the broadest range of care for patients with routine health care needs and those with complex and rare conditions. We accept referrals from across the region, using technology unavailable at other hospitals. Because of our educational and research missions, UTMB provides highly specialized and cutting-edge services, including sometimes costly treatments for rare illnesses and serious injuries. We translate research discoveries into new patient treatments. As a teaching hospital, we believe that we have an obligation to work with our referral hospitals to help “raise the bar” for health care in the state.
Like many other academic health systems, UTMB is also considered an “essential hospital”, which means we are dedicated to providing high-quality care for all, including uninsured, underinsured, and other vulnerable patients. These patient populations often have limited access to routine primary health care. For example, silent health problems, such as hypertension and diabetes, often go undetected without routine check-ups. Several consequences can result from limited access to care: these patients are often very ill by the time they require hospitalization, because they are diagnosed at late stages in a disease process; they are hospitalized more frequently, because they do not receive timely preventive care or participate in disease management programs; and/or they may be admitted to the hospital with more than one illness at a time.
It is important to note websites that currently exist on the internet and provide information on hospitals across Texas and the nation, such as Hospital Compare (www.medicare.gov/hospitalcompare), compare hospitals’ data reports under the assumption that all hospitals are similar. In reality, reporting methods on these “all-inclusive” hospital quality websites cannot account for all meaningful differences that influence hospital care.
+/- What are "pay-for-peformance" programs?
What are "pay-for-peformance" programs?
+/- What are the limitations of healthcare data reports?
What are the limitations of healthcare data reports?
Some public reports of health care provider and hospital performance rely solely on clinical documentation in the medical record. As such, these reports are sometimes a better index of how well the care delivered has been documented rather than how well they provided care.
Clinical documentation is “coded” for purposes of billing. Because of this, drawing conclusions about the quality of care from billing data is sometimes suspect (i.e., it is not the actual language used, and therefore may not be as comprehensive as what was written in the documentation). There has been significant support for the wide use of electronic medical records to reduce the reliance on billing data.
Quality measurement is not yet an exact science. Adjustments for severity of patient illness, while helpful, do not include characteristics such as:
- How sick the patient was when they arrived at the hospital
- What sort of lifestyle choices the patient made, such as how healthy they were eating or whether they were a smoker.
- What types of access a patient had to health care before they arrived at the hospital
- How well the patient understands what a healthy lifestyle is or basic medical terminology
Because of factors like these, professionals who measure patient outcomes use a method called risk adjustment or severity adjustment that “levels the playing field” when making comparisons between hospitals or health care providers.
When looking at quality outcomes for academic medical centers, it is important to note that because these “essential hospitals” provide charity care, they often receive patients who are very sick or did not take good care of themselves. The reason for this is that often, patients with very low incomes do not have access to health care services or will not go to a doctor until they are very sick.
When it comes to costs, comparisons can be misleading if they do not take into account the types of patients a hospital serves or the specialized nature of treatment and technology offered.
Results for different patient care outcomes sometimes vary from reporting period to reporting period. This is not only because the care the provider delivered varied, but because they may have been treating patients with co-existing conditions or complications (for example, individuals with a chronic illness, like diabetes, or a patient with nutritional deficiency can be more difficult to treat). In addition, patients who do not have a support system to help them after they are discharged from the hospital can may not heal as well as a patient who does.
Risk adjustment is a statistical process for reducing, removing, or clarifying the influences of confounding factors that differ among comparison groups. When including performance information about several hospitals or health systems in a single presentation, it is important to make the comparisons as fair as possible by making appropriate adjustments to published numbers. In the health care industry, this is usually called an adjustment for either risk, severity, or acuity. Making such numeric adjustments is a means of taking into account:
- average age of patients who share the same diagnosis (presumes that advancing age is associated with more involved disease or concurrent health problems),
- gender,
- the degree of medical morbidity (involvement of disease) for a patient,
- risk that a patient might die (mortality) or
- develop known (predictable) complications of medical treatment.
- What is severity adjustment and why is it important?
- because some patients are sicker than others and may therefore be more likely to have adverse outcomes or complications, hospital outcomes are said to be adjusted for the severity of their patients’ illnesses.
- psychosocial risk of health treatment or the
- degree of dependency or functional status of the patient.
