 A message from Dr. Gerald Beathard, the father of Interventional Nephrology
A message from Dr. Gerald Beathard, the father of Interventional Nephrology
History of Interventional Nephrology
Beginning in the 1980s and 1990s, dialysis access came to be recognized as a major problem, contributing to patient morbidity and mortality. Care of the vascular access was being placed in the hands of consultants where cases were often given a low priority,
resulting in delayed treatment, frequent hospitalizations, and an excessive use of central venous catheters. The desire to improve dialysis patient care, concerns for the welfare of dialysis patients, and an unwillingness to accept the status quo
gave rise to an interest and involvement in the planning and management of dialysis access starting in the mid-1980s. This activity, beginning in the private practice setting, proved to be effective and gave rise to a new subspecialty of nephrology
referred to as Interventional Nephrology.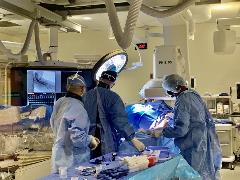
Initially, training in this new subspecialty was limited to the private practice setting and consisted of a few weeks of proctored activity. Beginning in the late 1990s, academic centers began to initiate programs in interventional nephrology. Some programs
engaged in a full range of hemodialysis and peritoneal dialysis access management procedures while others took a more limited approach.
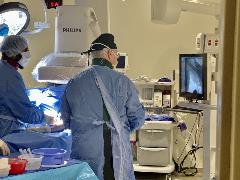 Early
reports from interventional nephrologist presented data documenting the success of procedure performed and the incidence of procedure related complications with results superior to that previously reported by other specialties from smaller studies.
These publications led to increasing numbers of nephrologists becoming involved in the subspecialty.
Early
reports from interventional nephrologist presented data documenting the success of procedure performed and the incidence of procedure related complications with results superior to that previously reported by other specialties from smaller studies.
These publications led to increasing numbers of nephrologists becoming involved in the subspecialty.
In 1996, the National Kidney Foundation annual meeting featured a workshop on kidney ultrasonography and dialysis catheter placement. This was followed in 1997 by the publication of the first iteration of the National Kidney Foundation Dialysis Outcome
Quality Initiative with an emphasis on vascular access. In 1998, the first of a series of Interventional Nephrology pre-courses was conducted at the annual American Society of Nephrology meeting. The professional society of interventional nephrology,
the American Society of Diagnostic and Interventional Nephrology (ASDIN), was formed in 2000 and Interventional Nephrology has become recognized by both the American Society of Nephrology and the Renal Physicians Association. Since that time, ASDIN
has developed practice guidelines, offered Interventional Nephrology certification and accreditation for training programs, and conducted Annual Scientific Meetings focused on dissemination of ongoing research and clinical expertise in vascular access.
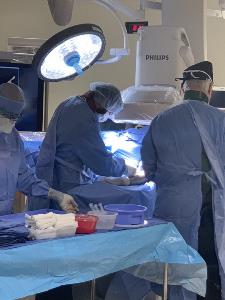
Today the management of dialysis access by nephrologists has come to be recognized as a standard of care and the subspecialty of Interventional Nephrology has become recognized worldwide.
The Interventional Nephrology Program at UTMB
A major component of nephrology practice is the management of patients with end-stage kidney disease (ESKD). A critical aspect of the care provided to this category patients is the planning of the dialysis access. Patients with ESKD represent a diverse
group requiring individualization based upon a detailed knowledge and understanding not only of the patient’s disease process, but also of the alternatives available including hemodialysis and peritoneal dialysis access.
Dialysis access planning and management requires a collaborative effort of a coordinated team including the patient and the multi-specialty healthcare professionals involved. It is important that the nephrologist play a pivotal role as the leader of this
team; however, in order to do so they must have a detailed knowledge of dialysis access planning and management.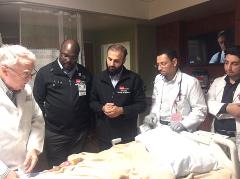
Core dialysis access knowledge must be an integral part of the nephrology training experience. The goal of the UTMB nephrology training program is to instill in the trainee a robust knowledge and experience in dialysis access through didactic sessions
and hands-on exposure. This will include access planning, access monitoring and surveillance, and access management. Each trainee will have the opportunity to participate in the activities of the interventional nephrology section of the nephrology
division. This will include training directed toward clinical competence in the placement of both acute and tunneled dialysis catheters as well as percutaneous kidney biopsies. Interventional nephrology will also be available as an elective which
will provide the opportunity for participation in endovascular procedures.