Watch Dr. Walser's laser treatment video
here.
Patients interested in laser ablation prostate treatment at UTMB can call (409) 747-4667 or email Dr. Walser or visit Wavelength Medical
A new non-surgical prostate cancer treatment offered at the University of Texas Medical Branch virtually eliminates the side effects of impotence and incontinence that can occur when patients receive the traditional treatment for prostate cancer - surgical
prostate removal.
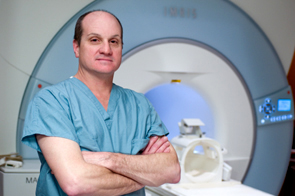
Dr. Eric Walser, is one of only a few physicians in the world and the only physician in Texas who performs this groundbreaking procedure. Using a state-of-the-art, MRI-guided laser ablation instrument developed at UTMB,
he zaps away the cancer without removing the prostate.
With national standards for prostate cancer screening changing so dramatically over the past year, many men are confused about what it means to have prostate cancer, whether they should be tested for it and what they should do if they test positive.
The American Urological Association released new prostate cancer screening guidelines saying men under 55 should no longer receive routine prostate screening and that men over 80 should not receive it if they have a life expectancy less than 10 to 15
years. The association determined the odds of preventing prostate cancer death with a PSA (prostate specific antigen) blood test for men ages 55 to 69 amounted to one life spared for every 1,000 men screened over a decade.
This is on the heels of the U.S. Preventive Services Task Force’s statement last May, saying that much more harm than good was being done to men who underwent screening, biopsy and surgical removal of their prostate gland. The vast majority of prostate
cancers are so slow-growing that they will never cause a problem. On the other hand, the impotence and incontinence that can result when the sensitive nerves surrounding the prostate are damaged or severed during surgery can be devastating.
The gist of all this is that the standard treatment - surgical prostate removal - causes more damage than the disease ever would have.
"The problem is, most men who test positive, even if the risk is one in 1,000 of dying of prostate cancer," said Walser, "still just want to get it out of there. You never know if you are going to be that one."
In the past, there was no way for doctors to remove prostate cancer without removing the whole prostate gland. This is because the available imaging technology was not powerful enough to illuminate the cancer and the available laser ablation technology
was not focused enough to remove the cancer without damaging surrounding tissue. But in recent years, the technology has improved significantly.
"Our approach pairs the most advanced MRI imaging to identify cancer-suspicious areas in the prostate and the most advanced laser technology to remove it completely, with virtually no risk of impotence or incontinence," said Walser.
Walser, who has been performing this procedure for over ten years, says this new way of treating prostate cancer offers selected men much more peace of mind than active surveillance or "watchful waiting", the traditional alternative to radical treatment.
Active surveillance is an invasive method to follow these patients and involves blood draws and often multiple prostate biopsies repeated yearly. "Watchful waiting" is less invasive but requires monitoring of patient symptoms and repeated transrectal
clinical exams. Neither method actually treats cancer in the prostate. Additionally, prostate MRI images may be able to separate aggressive from very slow growing prostate cancers and help physicians identify men needing earlier treatments.
NIH-funded clinical trials of this new procedure so far show that it is safe and effective, with results from several trials just published online in the journal Radiology and an ongoing study being conducted at the University of Chicago Medical school.
The Newest Innovations in Prostate Treatment
A new treatment for prostate cancer uses ultrasound beams. The treatment uses
ultrasound technology to eliminate cancer but leaves surrounding, healthy tissue unharmed. Watch video here.
The latest TULSA procedure at UTMB can be seen here.
For those patients whose prostate cancer is large, aggressive or has spread outside of the pelvis, ablation therapy may not be able to fully eliminate it. In those cases, UTMB’s Department of Urology offers the patient a wide range of minimally invasive surgical options, including a highly advanced robotically-assisted laparoscopic option for prostate removal. UTMB’s radiation oncology department also has methods to treat prostate cancer with focused radiation therapy.